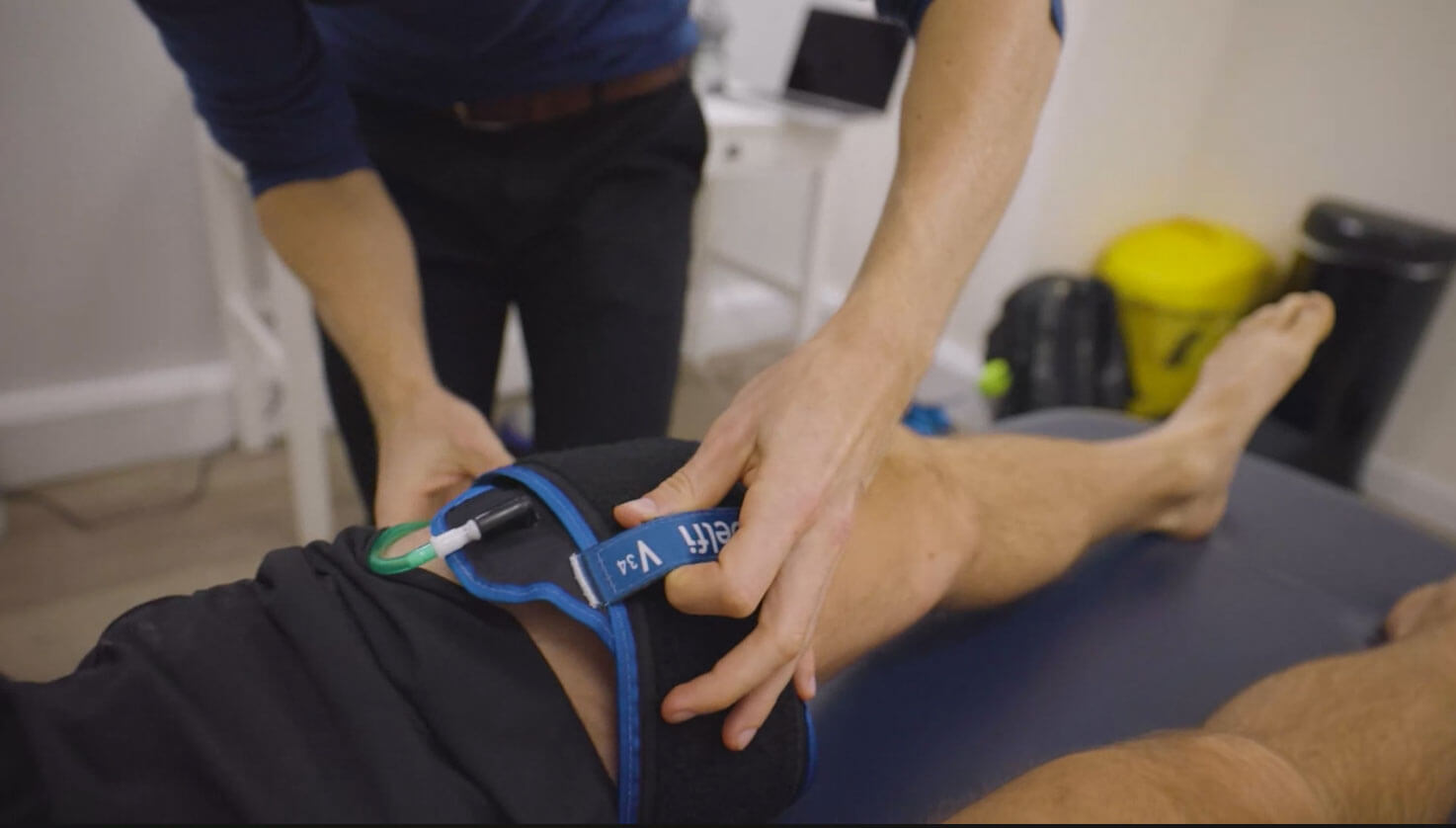
Complete Physio’s Blood Flow Restriction Training (BFRT) Service offers BFRT to enhance rehabilitation from injury, post-operative rehabilitation and for general health and well-being.
Headed by Rehabilitation Physiotherapist, Reece Noble, this service forms part of Complete Physio’s comprehensive offering of health care services.
This article covers the following areas
- Introduction to BFRT
- What BFRT can be used for
- Comparison of BFRT to High Load Resistance Training
- Why light loads may be chosen over heavy loads
- How long BFRT takes to work
- The physiological benefits of BFRT
- What a session of BFRT involves
- Safety of BFRT
- Is BFRT right for you?
What is Blood Flow Restriction Training?
Blood Flow Restriction Training (BFRT), which is also commonly referred to as occlusion training or KAATSU (Japanese for “additional pressure”) training, is a specific form of exercise therapy used by physiotherapists, doctors and other health professionals in both rehabilitation and for general health improvement.
BFRT was invented in Japan by Dr Yoshiaki Sato in the 1960’s who called it KAATSU training. Since then there has been almost 50 years of academic research and development of BFRT, with over 400 peer reviewed articles showing its positive effects.
BFRT involves applying a medically approved pneumonic cuff, similar to the one used to take your blood pressure, to moderately but safely restrict the blood flow in and out of a limb and performing light exercise with that limb. This leads to blood and metabolites pooling in the limb, triggering a cascade of beneficial physiological effects.
The main aim of BFRT is to induce hypertrophy (hypertrophy = muscular growth), and it has shown to be very effective at achieving this [1]. Hypertrophy is important because a bigger muscle means a stronger muscle, and strength is vital for almost all parts of life, not just for injury rehabilitation or when recovering from injury.
Whilst hypertrophy is generally the main aim of BFRT, it has a wide variety of physiological benefits beyond this, these benefits will be discussed further below [2].
What conditions and other health benefits can BFRT be used for?
BFRT can be utilised by health and rehab professionals to directly treat and in the treatment of a range of conditions and to achieve better general health outcomes. Some of these are;
- Post-surgical rehabilitation [3-14]
- Anterior Knee Pain (PFJP, Patella Tendinopathy) [15-18]
- Sarcopenia (age related loss of muscle mass)[19-26]
- Sports injury Rehabilitation [27-29]
- Strengthening for the management of
- Arthritis [15, 30-33]
- Osteoporosis/Osteopenia [34-38]
- Negate the negative effects of bed rest/immobilisation [12, 19, 39]
- Bone Fracture and Stress Injury Rehabilitation [19, 34-36, 40-42]
- Increased VO2 Max in elderly and athletic populations [24, 43-46]
- Improve vascular health/Circulation (Particularly in the elderly/aging population)[23, 25, 26, 47-52]
- Reduced risk of blood clots [25, 53, 54]
- Cardiac Rehab [55-57]
- Load management in athletes [58-61]
- Recovery post sports [62-64]
- Pre-Exercise Analgesia (pain reduction) [17, 65, 66]
- Ischemic preconditioning (preparing for exercise) [67, 68]
- Muscular gain for general health [20-26, 39, 41, 44, 60, 61, 69-81]
- Body Building [20-26, 39, 41, 44, 60, 61, 69-81]
- Diabetes management*
- Falls Prevention**
- Prevention of scar tissue formation***
*Increased muscle mass leads to reduced insulin resistance [82, 83]
** BFRT has been show to improve 30 second sit-stand test which is positively associated with reduced falls risk [25, 30, 31, 84-86]
*** BFR leads to down regulation of Myostatin which is a key step in scar tissue formation [87, 88]
Blood Flow Restriction Training vs High Load Resistance Training – same outcomes without the weight
Traditionally, high load resistance training (HLRT) is used to improve muscular strength and hypertrophy. Ultimately, by lifting heavy things our muscles will get stronger[89].
Where BFRT has great advantage over HLRT, is that hypertrophy and other beneficial health effects are able to be achieved using very light loads and in a short amount of time [2].
Simply put, BFRT = quick strength gains with low loads
Why would we only want to use light loads? This is to protect healing, compromised or sensitive tissue from injury which can occur by using too heavy a load.
We refer to a person with tissues described above as being “load compromised”, meaning they can’t handle heavy loads. A few examples of this are after surgery (e.g. ACL reconstruction), when a tissue is healing (e.g. a broken leg) or if a joint is degenerated (e.g. an arthritic knee).
Why not just use light loads by themselves?
A fair question to ask is why not just use light loads to achieve hypertrophy? Unfortunately, use of light loads alone does not cause enough stress to stimulate muscular hypertrophy [89].
To understand this better, it is helpful to know the two ways our body makes our muscles grow. These are in response to mechanical stress and metabolic stress [89].
- Mechanical stress, caused by lifting heavy loads above 70%+ of 1RM (1 RM = the maximum weight you can lift once),
- This leads to micro damage of muscle tissue. Micro damage is completely normal and when followed by natural healing, i.e. “Breaking down and building up”, leads to a bigger muscle.
- Blood pooling insode the limb stimulates the mTOR pathway – which is a pathway that stimulates the brain to upregulate protein synthesis – i.e. start building muscle
- Metabolic Stress is caused by a build-up of metabolites, which are natural chemicals, that our cells release in response to high intensity exercise (i.e. lifting heavy). These chemicals then stimulate the body to grow muscle.
Use of light loads alone does not cause enough of either of these stresses to stimulate the body to grow muscle.
How does the addition of Blood Flow Restriction make light loads stimulate hypertrophy?
BFRT is able to achieve increases in strength, but without the need for heavy loads predominantly by stimulating hypertrophy through metabolic stress pathways, along with sell swelling caused by blood pooling activating the mTOR pathway [90].
By restricting blood flow and using light loads during BFRT (lifting light or, in the very early stages of rehab, this exercise may be as light as walking or riding a bike with BFR), we deprive the working muscles of oxygen which leads to a build-up of metabolites & cell swelling in the working limb.
The hypoxic (low oxygen) environment also causes the Type II muscle fibres (strength fibres) to contract instead of type I fibres (endurance fibres).
This mimics what would occur using traditional HLRT, without mechanical force on the working tissues, meaning it safe for the tissues when load compromised.
Basically – your body gets tricked into working hard using a light load, which makes BFRT a fantastic tool to build strength, particularly in a rehabilitation setting.
Why not use BFRT instead of high load resistance training all the time?
A question that is often asked is “why would we not use BFRT in preference to HLRT all the time?”, there are two main reasons for this.
Firstly, if we look beyond just muscular strength, other tissues in our body, namely tendon and bone, require mechanical loading to build up strength and stay healthy. Utilisation of HLRT induces beneficial changes in bone and tendon health that BFRT cannot [91, 92].
On top of the benefit to tendon and bone, most studies show that HLRT leads to strength gains of 1.3-1.6x greater than BFRT [31, 35, 38, 41, 61, 71, 73, 77, 79, 93, 94], so to reach maximum levels of strength, HLRT is advised.
This is a consideration when rehabbing or preparing athletes for high level performance, where max strength is an important attribute.
In most cases, but not always, the goal is to progress onto HLRT. BFRT plays a vital role in starting rehabilitation and more specifically, building strength, much earlier than what otherwise could have without BFRT.
This also makes the commencing HLRT easier to achieve and it can be started at a much higher level, reducing overall rehabilitation times and improving outcomes.
How long does BFR take to work?
Improvement in muscular hypertrophy and strength can generally be seen after 2 weeks using BFRT, this is in comparison to traditional HLRT that takes 8-12 weeks to see improvements.
The reason for this difference is that strength gains seen using BFRT are driven by changes in the muscle tissue itself (i.e. hypertrophy) [95] whereas strength gains seen with traditional HLRT are driven by the nervous system for the first 8 weeks then hypertrophy takes over after that [89].
This is often taken into consideration when rehabilitating an athlete that needs to get back to performing very quickly.
The many physiological benefits of BFRT (it’s more than just hypertrophy)
Whilst hypertrophy has traditionally been the main aim of BFRT, a number of other physiological benefits have been discovered to be induced by BFRT
These are angiogenesis (growth of new blood vessels) [47], analgesia (pain reduction) [65, 66], reduced autophagy (tissue break down) [55, 80] and improvements in VO2 max (cardiovascular health) [43]
What does a session of Blood Flow Restriction Training involve? – the practical side
A session of BFRT will be different depending on a number of factors including what injury you have, what your goals are, your general health and how much training you have done in the past. This will be tailored to you by your physiotherapist to ensure it is effective and safe.
There are 3 ways we use BFRT, BFR + Resistance Training (BFR-RT), BFR + Aerobic Exercise (BFR-AE) and Passive BFR a thorough description of each and their applications can be found here.
In clinic BFR-RT and BFR-AE are the most common applications and a session will follow these steps;
- Safety checks
- make sure it is safe to conduct the session
- Find Arterial Occlusion Pressure (AOP)
- AOP = amount of pressure the cuff is inflated to that stops arterial blood flow into the limb
- This is the same as your systolic blood pressure (the higher number on a blood pressure reading)
- May not occur every session – commonly rechecked every 1-4 weeks
- Determine what % of AOP training will occur at
- Up to 50% is used in the arm and 80% is used in the leg
- Early in training lower pressures are used and then advanced
- These pressures allow blood to flow into the limb, but not out, which leads to the all-important pooling.
- Commence the exercise
- BFR-RT
- Lift a load 30% or less of 1RM
- 75 reps in sets of 30/15/15/15 with 30 seconds rest between
- Load will be advanced over time
- FR-AE
- Undertake aerobic exercise for a set amount of time
- Commonly begins at 5 minutes and is progressed from there
- BFR-RT
- Cuffs are deflated
- If a second round of BFR is to be conducted within the same session
- 5 minutes rest if exercising the same limb
- Commence immediately if exercising a different limb
- If a second round of BFR is to be conducted within the same session
Is BFRT Safe?
As with any therapeutic or fitness intervention, safety must be the first consideration before undertaking BFRT. Overall, BFRT has been shown to be very safe, just as safe as regular strength training in fact [96, 97].
But there are some people that cannot use BFRT, here’s a list of common conditions that may exclude someone from being able to use BFRT.
- Unstable Cardiac Disease
- Active or recent blood clots including Deep Vein Thrombosis (DVT)
- Severe varicose veins
- Pregnancy
- Active infection
- Wounds
The BIG question – does BFRT increase the risk or cause blood clots?
As BFRT causes blood to pool inside the limb, a common question is about the risk of thrombogenesis (blood clots) or DVT whist using BFRT.
Current evidence suggests that there is no increased risk of blood clots or DVT whilst using BFRT, in those that do not already show signs or risk factors of clotting or DVT [3].
Blood clots are caused by 3 factors, known as “Virchow’s Triad”. 1. Stasis (stagnant blood), usually through inactivity, such as bed rest or long-haul travel, 2. Hypercoagulation (excessively easy clotting of the blood) and 3. Endothelial (Blood Vessel) damage [98].
Whilst BFRT does lead to partial stasis in the limb, the lack of complete occlusion by only using a % of AOP and also the short time BFRT is used (usually 8 minutes) ensures stasis is not to a level to induce coagulation. Patients will be assessed for the two other factors. Further to this BFRT does not show an increase of markers of thrombogenesis in the blood [57].
In fact, there is emerging evidence that BFRT is protective against blood clots and DVT through the release of Tissue Plasminogen Activator (tPA) which is a protein involved in the break-down of blood clots [54] and also by improving vein health [47-50, 52].
All patients will be screened by a health care professional prior to any BFRT to assess if it is appropriate and safe for them to undertake.
How do I know if BFRT is right for me?
The best way to assess if BFRT is appropriate to be used in your rehabilitation or general health care is to contact a physiotherapist or health care provider qualified in Blood Flow Restriction Training.
Also, here are some further articles written by Compete Physio team members on BFRT
Complete Physio’s BFRT is led by Rehabilitation Physiotherapist Reece Noble. Reece works from our physiotherapy clinics on Fulham Road (Chelsea clinic) and the city (Broadgate clinic).
For more information or book in for a physio assessment to find out if BFRT is an option for you, please email Reece direct on reece@complete-physio.co.uk.
References
1. Lambert, B.S., et al., Blood Flow Restriction Therapy for Stimulating Skeletal Muscle Growth: Practical Considerations for Maximizing Recovery in Clinical Rehabilitation Settings. Techniques in Orthopaedics, 2018. 33(2): p. 89-97.
2. Jessee, M.B., et al., Mechanisms of blood flow restriction: the new testament. Techniques in Orthopaedics, 2018. 33(2): p. 72-79.
3. Bond, C.W., et al., Blood Flow Restriction Resistance Exercise as a Rehabilitation Modality Following Orthopaedic Surgery: A Review of Venous Thromboembolism Risk. journal of orthopaedic & sports physical therapy, 2019. 49(1): p. 17-27.
4. DePhillipo, N.N., et al., The role of blood flow restriction therapy following knee surgery: Expert opinion. Arthroscopy: The Journal of Arthroscopic & Related Surgery, 2018. 34(8): p. 2506-2510.
5. Hughes, L., et al., Comparison of the acute perceptual and blood pressure response to heavy load and light load blood flow restriction resistance exercise in anterior cruciate ligament reconstruction patients and non-injured populations. Physical Therapy in Sport, 2018. 33: p. 54-61.
6. Hughes, L., et al., Blood flow restriction training in clinical musculoskeletal rehabilitation: a systematic review and meta-analysis. Br J Sports Med, 2017. 51(13): p. 1003-1011.
7. Hughes, L., et al., Examination of the comfort and pain experienced with blood flow restriction training during post-surgery rehabilitation of anterior cruciate ligament reconstruction patients: A UK National Health Service trial. Physical Therapy in Sport, 2019. 39: p. 90-98.
8. Hughes, L., et al., Comparing the Effectiveness of Blood Flow Restriction and Traditional Heavy Load Resistance Training in the Post-Surgery Rehabilitation of Anterior Cruciate Ligament Reconstruction Patients: A UK National Health Service Randomised Controlled Trial. Sports Medicine, 2019. 49(11): p. 1787-1805.
9. Hughes, L., et al., Blood flow restriction training in rehabilitation following anterior cruciate ligament reconstructive surgery: A review. Techniques in Orthopaedics, 2018. 33(2): p. 106-113.
10. Ohta, H., et al., Low-load resistance muscular training with moderate restriction of blood flow after anterior cruciate ligament reconstruction. Acta Orthopaedica Scandinavica, 2003. 74(1): p. 62-68.
11. Patterson, S.D., L. Hughes, and J. Owens, Early Postoperative Role of Blood Flow Restriction Therapy to Avoid Muscle Atrophy, in Return to Sport after ACL Reconstruction and Other Knee Operations. 2019, Springer. p. 261-274.
12. Takarada, Y., H. Takazawa, and N. Ishii, Applications of vascular occlusion diminish disuse atrophy of knee extensor muscles. Medicine & Science in Sports & Exercise, 2000. 32(12): p. 2035-2039.
13. Tennent, D.J., et al., Blood flow restriction training after knee arthroscopy: a randomized controlled pilot study. Clinical Journal of Sport Medicine, 2017. 27(3): p. 245-252.
14. Yow, B.G., et al., Blood flow restriction training after Achilles tendon rupture. The Journal of Foot and Ankle Surgery, 2018. 57(3): p. 635-638.
15. Bryk, F.F., et al., Exercises with partial vascular occlusion in patients with knee osteoarthritis: a randomized clinical trial. Knee Surgery, Sports Traumatology, Arthroscopy, 2016. 24(5): p. 1580-1586.
16. Giles, L., et al., Quadriceps strengthening with and without blood flow restriction in the treatment of patellofemoral pain: a double-blind randomised trial. British journal of sports medicine, 2017. 51(23): p. 1688-1694.
17. Korakakis, V., R. Whiteley, and K. Epameinontidis, Blood Flow Restriction induces hypoalgesia in recreationally active adult male anterior knee pain patients allowing therapeutic exercise loading. Physical Therapy in Sport, 2018. 32: p. 235-243.
18. Korakakis, V., R. Whiteley, and G. Giakas, Low load resistance training with blood flow restriction decreases anterior knee pain more than resistance training alone. A pilot randomised controlled trial. Physical Therapy in Sport, 2018. 34: p. 121-128.
19. Hackney, K.J., et al., The role of blood flow restriction training to mitigate sarcopenia, dynapenia, and enhance clinical recovery. Techniques in Orthopaedics, 2018. 33(2): p. 98-105.
20. Abe, T., et al., Effects of low-intensity walk training with restricted leg blood flow on muscle strength and aerobic capacity in older adults. Journal of geriatric physical therapy, 2010. 33(1): p. 34-40.
21. Centner, C., et al., Effects of blood flow restriction training on muscular strength and hypertrophy in older individuals: a systematic review and meta-analysis. Sports Medicine, 2019. 49(1): p. 95-108.
22. Fry, C.S., et al., Blood flow restriction exercise stimulates mTORC1 signaling and muscle protein synthesis in older men. Journal of applied physiology, 2010. 108(5): p. 1199-1209.
23. Ozaki, H., et al., Effects of 10 weeks walk training with leg blood flow reduction on carotid arterial compliance and muscle size in the elderly adults. Angiology, 2011. 62(1): p. 81-86.
24. Ozaki, H., et al., Increases in thigh muscle volume and strength by walk training with leg blood flow reduction in older participants. Journals of Gerontology Series A: Biomedical Sciences and Medical Sciences, 2011. 66(3): p. 257-263.
25. Yasuda, T., et al., Muscle size and arterial stiffness after blood flow‐restricted low‐intensity resistance training in older adults. Scandinavian journal of medicine & science in sports, 2014. 24(5): p. 799-806.
26. Yasuda, T., et al., Effects of low-load, elastic band resistance training combined with blood flow restriction on muscle size and arterial stiffness in older adults. Journals of Gerontology Series A: Biomedical Sciences and Medical Sciences, 2015. 70(8): p. 950-958.
27. Blazey, P., Blood flow restriction: miracle return to play adjunct or therapy fad? 2018. 28. Kimbrell, K. Managing muscle strains via personalized blood flow restriction (PBFR). 2019 [cited 2020 02 June]; Available from: https://www.owensrecoveryscience.com/blog/managing-muscle-strains-via-personalized-blood-flow-restriction-pbfr/.
29. Ziyout, H.A., et al., Implementation of Blood Flow Restriction for Injury Rehabilitation in the Athletic Training Setting. 2019.
30. Ferraz, R.B., et al., Benefits of resistance training with blood flow restriction in knee osteoarthritis. Med Sci Sports Exerc, 2018. 50(5): p. 897-905.
31. Rodrigues, R., et al., Low‐load resistance training with blood flow restriction increases muscle function, mass and functionality in women with rheumatoid arthritis. Arthritis care & research, 2019.
32. Segal, N., M.D. Davis, and A.E. Mikesky, Efficacy of blood flow-restricted low-load resistance training for quadriceps strengthening in men at risk of symptomatic knee osteoarthritis. Geriatric orthopedic surgery & rehabilitation, 2015. 6(3): p. 160-167.
33. Segal, N.A., et al., Efficacy of blood flow–restricted, low-load resistance training in women with risk factors for symptomatic knee osteoarthritis. PM&R, 2015. 7(4): p. 376-384.
34. Bittar, S., et al., Effects of blood flow restriction exercises on bone metabolism: a systematic review. Clinical physiology and functional imaging, 2018. 38(6): p. 930-935.
35. Karabulut, M., et al., Effects of high-intensity resistance training and low-intensity resistance training with a vascular restriction on bone markers in older men. European journal of applied physiology, 2011. 111(8): p. 1659-1667.
36. Loenneke, J.P., et al., Blood flow restriction: rationale for improving bone. Medical hypotheses, 2012. 78(4): p. 523-527.
37. Pereira Neto, E.A., et al., Walking with blood flow restriction improves the dynamic strength of women with osteoporosis. Revista Brasileira de Medicina do Esporte, 2018. 24(2): p. 135-139.
38. Silva, J., et al., Chronic Effect of Strength Training with Blood Flow Restriction on Muscular Strength among Women with Osteoporosis. Journal of Exercise Physiology Online, 2015. 18(4).
39. Natsume, T., et al., Effects of electrostimulation with blood flow restriction on muscle size and strength. Medicine & Science in Sports & Exercise, 2015. 47(12): p. 2621-2627.
40. Beekly, M.D., Y. Sato, and T. Abe, KAATSU-walk training increases serum bone-specific alkaline phosphatase in young men. International Journal of KAATSU Training Research, 2005. 1(2): p. 77-81.
41. Kim, S., et al., Effects of short term low intensity resistance training with blood flow restriction on bone markers and muscle cross-sectional area in young men. International Journal of Exercise Science, 2012. 5(2): p. 6.
42. Bemben, D., et al., Effects of a single bout of low intensity KAATSU resistance training on markers of bone turnover in young men. International Journal of KAATSU Training Research, 2007. 3(2): p. 21-26.
43. Bennett, H. and F. Slattery, Effects of blood flow restriction training on aerobic capacity and performance: A systematic review. The Journal of Strength & Conditioning Research, 2019. 33(2): p. 572-583.
44. Abe, T., et al., Effects of low-intensity cycle training with restricted leg blood flow on thigh muscle volume and VO2max in young men. Journal of sports science & medicine, 2010. 9(3): p. 452.
45. Christiansen, D., et al., Cycling with blood flow restriction improves performance and muscle K+ regulation and alters the effect of anti‐oxidant infusion in humans. The Journal of physiology, 2019. 597(9): p. 2421-2444.
46. Kaijser, L., et al., Muscle oxidative capacity and work performance after training under local leg ischemia. Journal of Applied Physiology, 1990. 69(2): p. 785-787.
47. Hunt, J.E., et al., Time course of regional vascular adaptations to low load resistance training with blood flow restriction. Journal of applied physiology, 2013. 115(3): p. 403-411.
48. Iida, H., et al., Effects of walking with blood flow restriction on limb venous compliance in elderly subjects. Clinical physiology and functional imaging, 2011. 31(6): p. 472-476.
49. Larkin, K.A., et al., Blood flow restriction enhances post–resistance exercise angiogenic gene expression. Medicine and science in sports and exercise, 2012. 44(11): p. 2077.
50. Patterson, S.D. and R.A. Ferguson, Increase in calf post-occlusive blood flow and strength following short-term resistance exercise training with blood flow restriction in young women. European journal of applied physiology, 2010. 108(5): p. 1025-1033.
51. Patterson, S.D. and R.A. Ferguson, Enhancing strength and postocclusive calf blood flow in older people with training with blood-flow restriction. Journal of aging and physical activity, 2011. 19(3): p. 201-213.
52. Shimizu, R., et al., Low-intensity resistance training with blood flow restriction improves vascular endothelial function and peripheral blood circulation in healthy elderly people. European journal of applied physiology, 2016. 116(4): p. 749-757.
53. Madarame, H., et al., Effects of low‐intensity resistance exercise with blood flow restriction on coagulation system in healthy subjects. Clinical physiology and functional imaging, 2010. 30(3): p. 210-213.
54. Nakajima, T., et al., Effects of KAATSU training on haemostasis in healthy subjects. International Journal of KAATSU Training Research, 2007. 3(1): p. 11-20.
55. Curty, V.M., et al., Blood flow restriction attenuates eccentric exercise‐induced muscle damage without perceptual and cardiovascular overload. Clinical physiology and functional imaging, 2018. 38(3): p. 468-476.
56. Ishizaka, H., et al., Blood Flow Restriction Increases the Neural Activation of the Knee Extensors During Very Low-Intensity Leg Extension Exercise in Cardiovascular Patients: A Pilot Study. Journal of clinical medicine, 2019. 8(8): p. 1252.
57. Madarame, H., et al., Haemostatic and inflammatory responses to blood flow‐restricted exercise in patients with ischaemic heart disease: a pilot study. Clinical physiology and functional imaging, 2013. 33(1): p. 11-17.
58. Bjørnsen, T., et al., Type 1 Muscle Fiber Hypertrophy after Blood Flow–restricted Training in Powerlifter. 2018.
59. Hansen, S.K., et al., Effects of alternating blood-flow restricted training and heavy-load resistance training on myofiber morphology and mechanical muscle function. Journal of Applied Physiology, 2020.
60. Nielsen, J.L., et al., Proliferation of myogenic stem cells in human skeletal muscle in response to low‐load resistance training with blood flow restriction. The Journal of physiology, 2012. 590(17): p. 4351-4361.
61. Yasuda, T., et al., Combined effects of low-intensity blood flow restriction training and high-intensity resistance training on muscle strength and size. European journal of applied physiology, 2011. 111(10): p. 2525-2533.
62. Beaven, C.M., et al., Intermittent lower-limb occlusion enhances recovery after strenuous exercise. Applied Physiology, Nutrition, and Metabolism, 2012. 37(6): p. 1132-1139.
63. Dankel, S.J., et al., Post-exercise blood flow restriction attenuates muscle hypertrophy. European journal of applied physiology, 2016. 116(10): p. 1955-1963.
64. Page, W., R. Swan, and S.D. Patterson, The effect of intermittent lower limb occlusion on recovery following exercise-induced muscle damage: A randomized controlled trial. Journal of science and medicine in sport, 2017. 20(8): p. 729-733.
65. Ellingson, L.D., et al., Does exercise induce hypoalgesia through conditioned pain modulation? Psychophysiology, 2014. 51(3): p. 267-276.
66. Hughes, L. and S.D. Patterson, The effect of blood flow restriction exercise on exercise-induced hypoalgesia and endogenous opioid and endocannabinoid mechanisms of pain modulation. Journal of Applied Physiology, 2020. 128(4): p. 914-924.
67. Incognito, A.V., J.F. Burr, and P.J. Millar, The effects of ischemic preconditioning on human exercise performance. Sports medicine, 2016. 46(4): p. 531-544.
68. Marocolo, M., et al., Ischemic preconditioning and placebo intervention improves resistance exercise performance. The Journal of Strength & Conditioning Research, 2016. 30(5): p. 1462-1469.
69. Abe, T., C.F. Kearns, and Y. Sato, Muscle size and strength are increased following walk training with restricted venous blood flow from the leg muscle, Kaatsu-walk training. Journal of applied physiology, 2006. 100(5): p. 1460-1466.
70. Bowman, E.N., et al., Proximal, Distal, and Contralateral Effects of Blood Flow Restriction Training on the Lower Extremities: A Randomized Controlled Trial. Sports health, 2019. 11(2): p. 149-156.
71. Brandner, C.R., D.J. Kidgell, and S.A. Warmington, Muscular Adaptations to Whole Body Blood Flow Restriction Training and Detraining. Frontiers in physiology, 2019. 10: p. 1099.
72. Colomer-Poveda, D., et al., Effects of 4 weeks of low-load unilateral resistance training, with and without blood flow restriction, on strength, thickness, V wave, and H reflex of the soleus muscle in men. European journal of applied physiology, 2017. 117(7): p. 1339-1347.
73. Ellefsen, S., et al., Blood flow-restricted strength training displays high functional and biological efficacy in women: a within-subject comparison with high-load strength training. American Journal of Physiology-Regulatory, Integrative and Comparative Physiology, 2015. 309(7): p. R767-R779.
74. Fahs, C.A., et al., Muscular adaptations to fatiguing exercise with and without blood flow restriction. Clinical physiology and functional imaging, 2015. 35(3): p. 167-176.
75. Lowery, R.P., et al., Practical blood flow restriction training increases muscle hypertrophy during a periodized resistance training programme. Clinical physiology and functional imaging, 2014. 34(4): p. 317-321.
76. Pearson, S.J. and S.R. Hussain, A review on the mechanisms of blood-flow restriction resistance training-induced muscle hypertrophy. Sports medicine, 2015. 45(2): p. 187-200.
77. Takarada, Y., et al., Effects of resistance exercise combined with moderate vascular occlusion on muscular function in humans. Journal of applied physiology, 2000. 88(6): p. 2097-2106.
78. Thiebaud, R.S., et al., The effects of elastic band resistance training combined with blood flow restriction on strength, total bone‐free lean body mass and muscle thickness in postmenopausal women. Clinical physiology and functional imaging, 2013. 33(5): p. 344-352.
79. Vechin, F.C., et al., Comparisons between low-intensity resistance training with blood flow restriction and high-intensity resistance training on quadriceps muscle mass and strength in elderly. The Journal of Strength & Conditioning Research, 2015. 29(4): p. 1071-1076.
80. Wilson, J.M., et al., Practical blood flow restriction training increases acute determinants of hypertrophy without increasing indices of muscle damage. The Journal of Strength & Conditioning Research, 2013. 27(11): p. 3068-3075.
81. Yasuda, T., et al., Effects of low‐intensity bench press training with restricted arm muscle blood flow on chest muscle hypertrophy: a pilot study. Clinical physiology and functional imaging, 2010. 30(5): p. 338-343.
82. Moon, S.-S., Low skeletal muscle mass is associated with insulin resistance, diabetes, and metabolic syndrome in the Korean population: the Korea National Health and Nutrition Examination Survey (KNHANES) 2009-2010. Endocrine journal, 2013: p. EJ13-0244.
83. Srikanthan, P. and A.S. Karlamangla, Relative muscle mass is inversely associated with insulin resistance and prediabetes. Findings from the third National Health and Nutrition Examination Survey. The Journal of Clinical Endocrinology & Metabolism, 2011. 96(9): p. 2898-2903.
84. Applebaum, E.V., et al., Modified 30-second Sit to Stand test predicts falls in a cohort of institutionalized older veterans. PloS one, 2017. 12(5).
85. Mattar, M.A., et al., Safety and possible effects of low-intensity resistance training associated with partial blood flow restriction in polymyositis and dermatomyositis. Arthritis research & therapy, 2014. 16(5): p. 473.
86. Yokokawa, Y., et al., Effects of low-intensity resistance exercise with vascular occlusion on physical function in healthy elderly people. Biosci Trends, 2008. 2(3): p. 117-123.
87. Järvinen, T.A., et al., Muscle injuries: biology and treatment. The American journal of sports medicine, 2005. 33(5): p. 745-764.
88. Laurentino, G.C., et al., Strength training with blood flow restriction diminishes myostatin gene expression. Medicine & Science in Sports & Exercise, 2012. 44(3): p. 406-412.
89. Schoenfeld, B.J., The mechanisms of muscle hypertrophy and their application to resistance training. The Journal of Strength & Conditioning Research, 2010. 24(10): p. 2857-2872.
90. Loenneke, J., G. Wilson, and J. Wilson, A mechanistic approach to blood flow occlusion. International journal of sports medicine, 2010. 31(01): p. 1-4.
91. Manske, S.L., C.R. Lorincz, and R.F. Zernicke, Bone health: part 2, physical activity. Sports Health, 2009. 1(4): p. 341-346.
92. Galloway, M.T., A.L. Lalley, and J.T. Shearn, The role of mechanical loading in tendon development, maintenance, injury, and repair. The Journal of bone and joint surgery. American volume, 2013. 95(17): p. 1620.
93. Lixandrão, M.E., et al., Effects of exercise intensity and occlusion pressure after 12 weeks of resistance training with blood-flow restriction. European journal of applied physiology, 2015. 115(12): p. 2471-2480.
94. Sieljacks, P., et al., Six weeks of low-load blood flow restricted and high-load resistance exercise training produce similar increases in cumulative myofibrillar protein synthesis and ribosomal biogenesis in healthy males. Frontiers in physiology, 2019. 10: p. 649.
95. Maughan, R., J.S. Watson, and J. Weir, Strength and cross‐sectional area of human skeletal muscle. The Journal of physiology, 1983. 338(1): p. 37-49.
96. Brandner, C.R., et al., Reported side-effects and safety considerations for the use of blood flow restriction during exercise in practice and research. Techniques in Orthopaedics, 2018. 33(2): p. 114-121.
97. Kacin, A., et al., Safety considerations with blood flow restricted resistance training. Annales Kinesiologiae, 2015. 6(1): p. 3-26.
98. Watson, T., E. Shantsila, and G.Y. Lip, Mechanisms of thrombogenesis in atrial fibrillation: Virchow’s triad revisited. The Lancet, 2009. 373(9658): p. 155-166.
Don’t let pain hold you back, book now!