What is it, do I have it and what can I do about it?
What is bursitis?
A bursa is a space between two adjacent anatomical structures to provide friction-free movement as they glide over each other. There are two bursae around the Achilles; the deep or retro-calcaneal bursa and the sub-cutaneneous or superficial bursa (see image below). When the bursa becomes inflamed and painful, they are known medically as a bursitis. A retrocalcaneal bursitis is more common than the sub-cutaneneous bursitis.
In our experience bursitis is one of the main reasons Achilles tendon problems fail to improve or fully resolve.
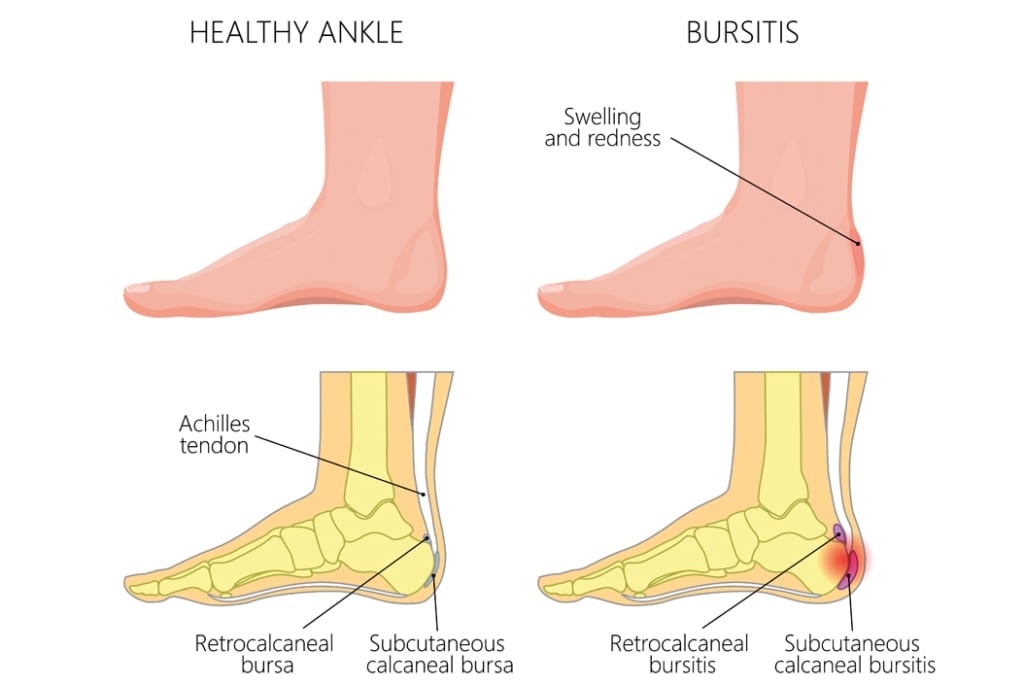
What is retrocalcaneal bursitis?
The retrocalcaneal bursa is a small space located between your Achilles tendon and the top of the heel bone (also known as the calcaneum). It is designed to reduce the friction between the tendon and the bone, created from repeated movements of your tendon as it moves over your calcaneus.
A normal bursa has a thin layer of synovial fluid within it. If the bursa is exposed to repeated compression or friction then the bursal lining becomes inflamed. This causes an increase in the amount of synovial fluid in the bursa. If this area is tender to touch and swollen on ultrasound, it is known as retrocalcaneal bursitis (Wilson et al, 2014). Retro-calcaneal bursitis is common in runners and footballers but is also prevalent over the age of 40 in less active individuals.

What causes retrocalcaneal bursitis?
Retrocalcaneal bursitis is often associated with an increased, inappropriate or unexpected mechanical stress (Buda et al, 2013). As previously discussed, this stress causes the bursa to come inflamed and painful.
Pain usually starts suddenly for various reasons:
- after undertaking a new form of exercise such as hiking or running
- increasing your training load too quickly
- wearing a new pair of shoes.
Trauma is not commonly associated with the onset of retrocalcaneal bursitis, you simply notice a sudden onset of sharp/burning or sometimes achy pain just above your heel. Some people report the sensation of squeaking accompanying this pain when ascending and descending stairs.
Retro-calcaneal bursitis is common in runners who are training for a marathon or have increased their training miles too quickly. We always advise that you do not increase your mileage too quickly. Remember the 10% rule; do not increase your mileage by more than 10% in one week.
What is sub-cutaneneous bursitis?
The sub-cutaneous bursa is more superficial (closer to the skin) located between the Achilles tendon and the skin. This is known as the superficial or sub-cutaneneous bursa. This can also become inflamed. If it is tender to touch and there is swelling in the bursa on ultrasound, it is known as a subcutaneous bursitis. Similarly this can occur in runners and those over 40.
What causes sub-cutaneneous bursitis?
The sub-cutaneneous bursa which is more superficial (closer to the skin) and normally begins after blunt trauma. The classic cause is being kicked or ‘studded’ in the heel by an opponent whilst playing football or rugby or a shopping trolley hitting your heel.
This is a very painful condition and often takes a long time to settle or requires an ultrasound-guided steroid injection to reduce the pain.
How is bursitis diagnosed?
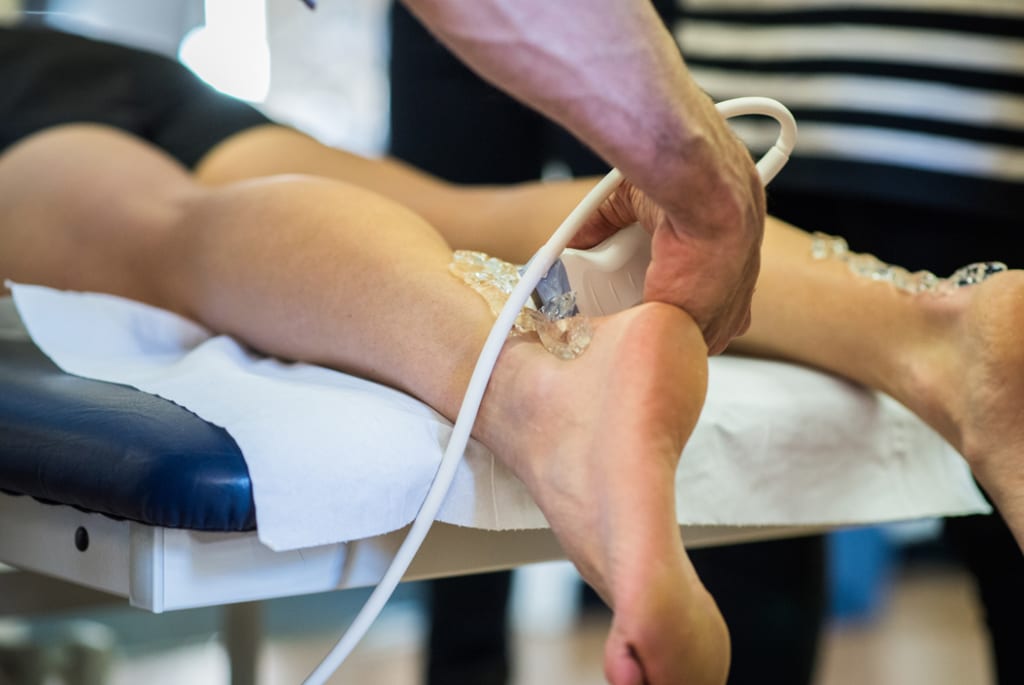
Obtaining an accurate diagnosis is critical. Clinical assessment cannot accurately diagnose a bursitis. If you want to know if you have a bursitis then you need to have a diagnostic ultrasound scan carried out. An MRI can also diagnose a bursa but this area is best visualised on ultrasound.
At Complete we have a team of highly experienced physiotherapists who are all fully qualified musculoskeletal sonographers. Your assessment will include a full clinical assessment as well as the ultrasound scan.
Ultrasound imaging is an effective assessment tool that is able to assess your bursa as well as ligaments, muscle and bony surfaces. We do not charge for an ultrasound at Complete. It is carried out as part of your assessment to ensure we get the right diagnosis before proceeding with a treatment plan.
Bursitis can often be mis-diagnosed or overlooked in the presence of Achilles tendinopathy or tendinitis. It does often co-exist with Achilles tendon issues and is a common reason why Achilles symptoms do not settle down with exercise alone.
What else could it be?
The other conditions that can present similar to a bursitis are:
- stress fracture of the heel
- Achilles insertional tendinopathy
- Posterior ankle impingement
- Peronal tendon tear or tenodinopathy
- Referred pain from the lower back (lumbar spine)
Clinical assessment and an ultrasound will rule in or out these other diagnoses for heel pain.
It is worth noting that Retrocalcaneal bursitis can also be an early sign of systemic inflammation such as rheumatoid arthritis (Suzuki et al, 2018). If your clinician is suspicious of this you may be asked to undertake blood tests via your GP or see a rheumatologist. This is rare but if you suffer with any other symptoms in the list below you should be assessed by your GP.
- Swollen, painful joints particularly if it effects both sides of the body e.g. both wrists
- Eye, bladder or bowel infections
- Skin rashes
- Family history of rheumatoid arthritis or ankylosing spondylitis
- If you generally feel unwell or always tired
How do we treat bursitis?

Bursitis usually responds well to conservative management. Physiotherapy treatment will depend on your individual assessment findings but may include soft tissue techniques and joint mobilisations. We may also advise you to purchase a heel raise to wear in your shoes or ‘off the shelf’ orthotics.
We are likely to also modify your training programme to ensure you do not irritate the area further. If you have poor foot posture, we may recommend you see a podiatrist for a more detailed assessment and to consider custom made orthotics.
Your physiotherapist will also prescribe an individualised exercise program which is likely to involve some strengthening exercises. We often find that stretches can actually further irritate the area.
Here are a few top tips you may like to try;
- An off-the-shelf orthotic/foot support OR a heel raise in your shoe to take the pressure off and allow the inflammation in your bursa to settle.
- Reduce your running and /or training load.
- Wear supportive shoes – tight leather slip-on shoes or flat shoes especially those with poor support e.g. Nike Free trainers or Converse All-Stars can aggravate these conditions.
- Calf strengthening exercises such as heel raises.
- Topical anti-inflammatory creams or patches, however, talk to your pharmacist first as some people are allergic to these.
What if conservative treatment doesn’t work?
If conservative options have been unsuccessful there are a few other treatment modalities available to you.
If there is a clear bursitis on ultrasound and the pain is persistent then an ultrasound-guided injection may be offered. We have had good success with steroid injections for those chronic stubborn retro-calcaneal and sub-cutaneneous Achilles bursitis. This needs to be discussed thoroughly with your clinician prior to undertaking as there is a small risk of tendon rupture. This is an extremely rare side effect (1 in 10,000) but needs to be considered prior to undertaking a bursal injection.
An ultrasound-guided injection consists of a mixture of local anaesthetic and corticosteroid (a potent anti-inflammatory). It is injected under the guidance of a real time ultrasound scan to ensure we target the bursa specifically. A steroid injection can give you rapid pain relief to provide a window of opportunity to continue with your rehabilitation. Our goal is to get you back to full function as quickly and as safely as possible, whether that is simply walking to work or running a marathon.
Complete has a team of highly experienced physiotherapists who use diagnostic ultrasound as part of their assessment to diagnose injuries and carry our ultrasound-guided injections. For further information please contact us on 020 7482 3875 or email info@complete-physio.co.uk.
Don’t let pain hold you back, book now!


