What’s the difference between Physiotherapy and Osteopathy?
What’s the difference between Physiotherapy and Osteopathy?
What’s the difference between Physiotherapy and Osteopathy, and which one should I see?
Have you ever asked yourself “What’s the difference between Physiotherapy and Osteopathy?” As both a qualified physiotherapist and registered osteopath, I am in an excellent position to try and answer this!
At Complete we have two dual trained physiotherapists and Osteopaths; myself (Chris Myers) and Francesco Contiero. We believe that this provides a unique set of assessment and treatment skills. Some may say you get the best of both worlds!
It is a common question that clients regularly ask, and I will endeavour to give you an insight into the main similarities and differences.
Origins and Philosophy
The origins and underlying philosophies of physiotherapy and osteopathy differ. However, if you read the “definitions” of physiotherapy and osteopathy, they sound remarkably similar.
This is not surprising as they essentially treat very similar conditions.
Physiotherapy helps people affected by injury, illness or disability through movement and exercise, manual therapy, education and advice. They maintain health for people of all ages, helping patients to manage pain and prevent disease (Chartered Society of Physiotherapists).
Osteopathy works with the structure and function of the body. It is based on the principle that the well-being of an individual depends on the skeleton, muscles, ligaments and connective tissues functioning smoothly together. Osteopaths use physical manipulation, stretching and massage to:
- increase joint mobility,
- relieve muscle tension,
- enhance the blood and nerve supply,
- and to help your body’s own healing mechanisms
(General Osteopathic Council).
I would suggest that although both professions do promote that they treat/manage all muscle and joint issues, osteopaths however predominantly treat more spinal problems such as lower back and neck pain.
Overall osteopaths treat fewer peripheral joints, e.g. the shoulder, wrist/hand, knee and ankle/foot.
Additionally, they treat less muscle and tendon related injuries than a physiotherapist. I would propose approximately 80% of most osteopath’s clinic list is spine related unless they have specialised in a particular area. Whereas physiotherapists’ training and experience expose them to a more varied caseload of both spinal, peripheral joint issues as well as muscle and tendon injuries.
Most of our physiotherapists see approximately 50% spinal and 50% peripheral joints including muscles and tendons. All of the research and treatment protocols into muscle and tendon problems are led by physiotherapists. Many of our physiotherapists at Complete have worked in sports clubs or sports governing bodies. They have significant experience and expertise in treating recreation and professional/elite sportspeople with tendon and muscle complaints.
It is important you are seeing someone who has significant experience in your condition. After 20 years of treating clients aches and pains, I know I get my best results with a condition I see regularly.
Always do your research on the therapist you plan to see and the clinic, before booking into a clinic.
Physiotherapy
The earliest documented origins of physiotherapy date back to Per Henrik Ling “Father of Swedish Gymnastics” in 1813 for soft tissue treatment, manipulation, and exercise.
Physiotherapy is a science-based, dynamic profession that is based on the best available evidence for treating and managing pain and movement.

I qualified as a physiotherapist 20 years ago and feel that over these years, the profession has evolved significantly to reflect the evidence and science that underpins musculoskeletal health. ‘Musculoskeletal’ refers to bones, muscles, fascia, tendons and ligaments. The scientific developments in pain and structure in the past 20 years have been substantial, and the profession has developed with these new emerging themes and theories.
Physiotherapy is much more aligned with Western medicine or the ‘Medical model’ than osteopathy.
Osteopathy
Osteopathy is a distinctive form of medical care. Founded on the philosophy that all body systems are interrelated and depending upon one another for good health. It is based on the work by Dr Andrew Still.
In 1874, a physician on the Missouri frontier, Andrew Taylor Still (image below) discovered that he could put his hands on people and change their physiology.

During my osteopathic study, I felt although these origins of osteopathy were fascinating to appreciate, on reflection, the profession was still based on outdated principles and had struggled to progress into a more modern evidence-based approach, especially to pain and dysfunction.
In the past few years, I believe this has started to change, and the profession has evolved, nevertheless it is still lacking the science that underpins its profession.
Training and Education
Both physiotherapy and osteopathy are undergraduate degrees (BSc Hons) studied at a university.
Physiotherapy is usually a 3-year degree and osteopathy a 4-year degree. Both degrees cover all the core subjects you would expect in the first few years; anatomy, biomechanics, physiology and pathology. As part of the degree, students’ complete clinical placements where they assess and treat real clients, providing the student essential experience in a clinic setting assessing, diagnosing and treating clients under the supervision of experienced, qualified clinicians.
Physiotherapists gain their experience in the NHS and osteopaths in a private teaching clinic affiliated with the university.
One of the key differences between the two degrees is the breadth of the medical conditions the clinician would be exposed to and expected to treat. As part of their university course physiotherapists attend work placements to put their skills into place and treat real patients. These are often in an NHS settings, hospitals, hospices, GP practices etc… and so work in a wide variety of health settings and treat a broad range of physical problems associated with different ‘systems’ of the body. Physiotherapists treat respiratory, neurological and musculoskeletal conditions. I believe this provides physiotherapists with an excellent foundation and range to their knowledge and skills.
Osteopaths also have clinical placements as part of their university course, however this is often a ‘private practice’ teaching clinic. Most patients will attend due to musculoskeletal pain and sports injuries e.g. neck and back pain. This exposes the osteopathy students to a narrower breadth of injuries and complaints during their training.
Assessment Process
During your first session, both a physiotherapist and osteopath will take a detailed clinical history and carry out a comprehensive assessment of your presenting condition. The overall assessment process is likely to appear quite similar. Still, there may be some differences depending on your individual therapist’s training and experience.
The assessment will involve the clinician asking you several questions and finding out about when and how your symptoms started and how the symptoms behave, i.e. what makes your pain better or worse. You will also be asked questions about your general health. The clinician will then go on and carry out a physical assessment of the affected area.
Generally, osteopaths probably assess a condition from a more holistic point of view, i.e. if you have a neck problem, they may assess your pelvis and lower limbs to see if these are contributing to your pain. They may even “assess” your internal organs; this is not something a physiotherapist would do.
Conversely, physiotherapists assess more locally to the painful or affected area but will also consider it as part of the overall functional unit. For example, if you have knee pain, a physiotherapist will assess the knee but will also evaluate the knee as part of a functional movement, e.g. a squat.
Many of our physiotherapists at Complete Physio are trained and qualified in the use of diagnostic ultrasound. Diagnostic ultrasound looks inside the body and allows the clinician to visualise a specific area, e.g. a joint, tendon or muscle and confirm the diagnosis. This takes away a significant amount of guesswork for the clinician. Very few osteopaths have developed this skill.
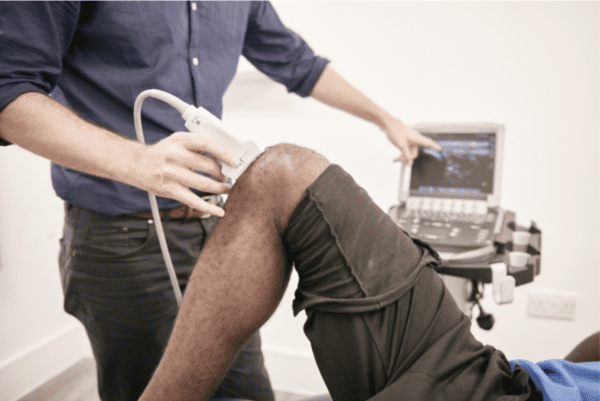
Chris carrying out a diagnostic ultrasound scan to diagnose a knee complaint.
Treatment
Obviously, the type of treatment you receive will depend very much on the individual therapist’s experience and training. Most physiotherapists will use a combination of ‘hands on’ treatment and exercise-based treatment (rehabilitation).
‘Hands on’ or manual therapy may involve techniques applied to your muscles and joints to improve their mobility and your overall range of motion.
It is very uncommon that you will see a physiotherapist that does not give you a home exercise-based programme. These exercises are aimed at reinforcing the benefits you have received in your treatment session and are an essential part of most treatment plans.
Osteopaths also use ‘hands on’ treatments but may not compliment this with exercises for you to carry out between your treatment sessions, making you more reliant on receiving their’ hands on’ treatment. This does vary from one clinician to another; however, most physiotherapists will use exercises as an essential part of their treatment regime more often than osteopaths.
During physiotherapists’ undergraduate training, there is more of a focus on the use of exercise therapy and rehabilitation. During my osteopathic education, there was very little of this, and I feel this is a critical limitation of osteopathic training. Many osteopaths do learn rehabilitation techniques but later in their training through postgraduate education.
A significant body of research has now been established to show exercise therapy is a very important part of a treatment program for any back condition. Certainly, all of the physiotherapists at Complete Physio have extensive postgraduate training in both manual therapy technique such as spinal manipulation combined with rehabilitation and exercise.
Physiotherapists also have extensive training and are exposed to the management and treatment of patients after operations such as ligament reconstructions, arthroscopies and back surgery. Osteopathic training does not expose you to this.
Post-operative rehabilitation
For post-operative rehabilitation, I would suggest you always see a physiotherapist. All of our physiotherapists have worked closely with orthopaedic surgeons for many years. They have managed clients from day 1 post-operation, ensuring they are pain-free when returning back to full function. Whether that be walking, playing football or their chosen sport…
Spinal manipulation
Another difference is the type of ‘hands on’ treatment you may receive. Spinal manipulation (high-velocity thrust techniques) is when a therapist’ cracks’ your spine or joint. The noise is actually gas bubbles being released from the joint. Both physiotherapist and osteopaths use spinal manipulation techniques, these can be very useful for treating acute low back pain and neck pain.
The origins of spinal manipulation are osteopathic, so you are more likely to receive this specific treatment if you see an osteopath. Spinal manipulation formed a significant part of my under-graduate osteopathic training and can be a useful technique for acute neck pain and stiffness, e.g. a wry neck.
Some physiotherapists will learn spinal manipulation as part of their postgraduate study. The key factor is that whoever you see for spinal manipulation, they must have extensive experience, and it is important you carry out some research beforehand.

As mentioned earlier, osteopaths often treat more holistically than physiotherapists. An osteopath may treat one part of the body to reduce pain in another. For example, they may treat your right shoulder pain by treating on your left hip. Additionally, osteopaths may assess and treat your internal organs, giving you specific nutritional and/or supplement advice. Particularly if they are a naturopath and osteopath (this combination is not uncommon).
Furthermore, some osteopaths will treat your internal organs, these are called visceral techniques.
For example, if you have irritable bowel syndrome (IBS) and lower back pain combined, an osteopath may treat your bowel specifically with ‘hands on’ techniques.
Physiotherapists would not carry out such techniques and are more likely to treat the local area affected.
Specialisms
Both osteopaths and physiotherapists will specialise in certain areas as they develop their experience and progress their interests and career. Due to the variety of specialisms within the professions, I would advise that you enquire about the skills and experience of the individual clinician you plan to see.
For example, at Complete Physio we have physiotherapists that specialise in:
- Pilates for low back pain and neck pain
- Rehabilitation post-operation
- Treatment of pre and post-natal conditions
- Shockwave therapy for tendon complaints
- Diagnostic ultrasound for the diagnosis of ligament tendon and muscle complaints
- Steroid injections to reduce pain
Many osteopaths also specialise in certain conditions or treatment techniques:
- Visceral (internal organs)
- Cranial-sacral, women’s health
- Paediatrics.
Conclusion
The reality is there are probably more similarities than differences!
It is not often related to whether your clinician is a physiotherapist or osteopath, but more their individual experience and training. I would always advise you to research your therapist before you see them or call their clinic to find out more information.
Francesco Contiero and Chris Myers are both dual trained physiotherapists and osteopaths and provide the ‘best of both’ approaches. At Complete we are always happy to speak to you before you book to answer any questions. This will help to ensure you find the right therapist for your specific problem.
If you would like an appointment to see Francesco or Chris please contact 020 7482 3875 or email info@complete-physio.co.uk

