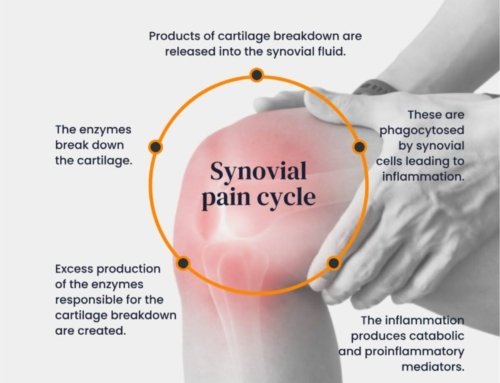
Delayed-union, non-union fractures and stress fractures
(Note: a ‘fracture’ is the same as a break or crack in the bone)
Focused shockwave is a safe, evidence-based treatment option for treating a wide variety of bony injuries. Focused shockwave delivers a series of powerful, rapid soundwaves directly to the site of injury where it excites the local tissues to stimulate a healing process. To improve bone healing a course of focused shockwave is required, consisting of between 3 to 8 sessions spaced one week apart.
This blog discusses what focused shockwave is, how it works and what it can treat. It also reveals the answers to our most frequently asked questions.
How does bone heal?
Bone healing can be divided into four stages and can take up to a year to complete. The four stages are described below:
- Day 1-5 – Immediately after the bone fractures the periosteum ruptures causing a bleed. This bleed forms a hematoma (a blood clot) which covers the fracture site. The job of the hematoma is to provide a quick fix and a subsequent scaffold for a callus to form.
- Day 5-11 – The hematoma is replaced by a fibrocartilaginous callus (a form of fibrous connective tissue). Chemicals within the hematoma start to lay down both collagen and osteoblasts which form a fibrocartilaginous callus.
- Day 11-28 – The fibrocartilaginous callus is converted into a bony callus. The fibrocartilaginous callus is slowly reabsorbed and replaced with calcium.
- Day 18 onwards – The bony callus is remodelled into compact bone. When the healing process is completed (in some cases up to a year) the fracture site returns to full bone.
Common bone injuries treated with focused shockwave
Delayed-union and non-union fractures
What are delayed-union and non-union fractures?
A full and healthy blood flow to the fracture site is of vital importance for effective healing to take place. When blood flow becomes impaired the fracture is unable to heal effectively, resulting in either a delayed-union or a non-union fracture (Schleusser et al., 2019).
Non-union fractures have been defined as fractures that persist for a minimum of 9 months without any sign of healing over 3 months (Li et al., 2021).
A delayed-union fracture simply means a fracture that is taking longer than expected to heal i.e., over 6 weeks.
Some bones, such as the scaphoid, have a complex and intricate blood supply which can easily be damaged after suffering a fracture. These bones are at a higher risk of developing a delayed-union or non-union fracture due to the higher risk of blood flow disruption post fracture.
The main symptom of a delayed-union or non-union fracture is ongoing pain for over 3 months. Delayed-union or non-union fracture is diagnosed using x-ray imaging and can be monitored with diagnostic ultrasound, MRI, or x-ray.
Stress fractures
What is a stress fracture?
Stress fractures are a common cause of lower limb pain in athletes and are responsible for up to 20% of all lower limb pathology in the sporting community (Roche et al., 2020).
A stress fracture is an overuse injury. If a bone is subjected to prolonged periods of repetitive, high impact forces, which it has not been gradually acclimatised to, then the bone’s structure and strength can become compromised. A compromised bone is unable to adequately repair itself and so becomes weakened. When a bone is unable to maintain its structure and strength the periosteum can become inflamed and swollen. The periosteum is a thin membrane which surrounds the bone. It is rich in blood and nerve endings and supplies the bone with both blood and sensation. An inflamed periosteum is known as periosteal oedema. If the bone is not rested, activities modified, and the aggravating activities stopped then a stress fracture can quickly follow (Leal et al., 2015). If caught early enough and the appropriate off-loading precautions are undertaken, a stress fracture will respond well to treatment. Unfortunately, research has revealed that up to one third of stress fractures do not respond to conservative treatment alone. Stress fractures which do not respond to conservative treatments are known as high stress fractures and may require surgery to stabilise (Leal et al., 2015). The goal of conservative treatment, focused shockwave included, is to stop a stress fracture becoming a high stress fracture, thereby avoiding surgical intervention.
Some stress fractures which do not respond to conservative treatments traditionally require surgery to stabilise (Leal et al., 2015). Focussed shockwave can provide an effective, simple non-surgical treatment option for stress fractures that do not heal or to facilitate the healing process.
Risk factors for developing a stress fracture include:
- Excessive amounts of high impact repetitive exercise without adequate training or rest periods.
- Low body mass index or BMI (a healthy BMI range is 18.5 to 24.9).
- Low bone density conditions such as osteopenia and osteoporosis (patients suffering from low bone density conditions are treated with bisphosphonate medication, HRT, and vitamin D supplements). Bone density can be assessed and monitored via a DEXA scan.
- Women have a higher rate of stress fractures than men.
- Poor biomechanics at the hip and foot can result in inappropriate loads through the leg, which can result in a stress fracture.
- Poor diet. Vitamin D and calcium are important in the development of bone and if not sufficiently present in the diet can result in weakened bones.
- Previous stress fracture. A history of stress fractures increases your risk of developing stress fractures in the future.
Symptoms associated with a stress fracture are:
- A deep aching pain felt directly over the site of the fracture.
- Pain when the bone is touched or knocked.
- Pain that gets worse with exercise and feels better with rest.
- Latent pain which manifests the day after exercise.
- Pain that gets worse over time. Pain often starts only with exercise, but over time can become constant, even at rest.
How are stress fractures diagnosed?
X-rays are routinely used to identify a stress fracture in A&E and hospitals. However, X-rays they often miss stress fractures especially if you have only had the pain for a few weeks. Periosteal oedema and small cracks (also known as fractures in the bone (often the first stage of stress fracture) can be well visualised on diagnostic ultrasound. However, the gold standard diagnostic tool for diagnosing stress fractures is MRI.
Focused shockwave
What is focused shockwave?
Focused shockwave is an evidence-based, non-invasive treatment modality capable of treating a wide variety of musculoskeletal conditions including stress fractures. Focused shockwave works by producing a series of short-lived but potent, high-pressure, acoustic pulses (Roche et al., 2020). These pulses cause a rapidly undulating rise and fall in pressure, causing a compressive/shear force on the underlying tissue. This undulation in pressure excites the cells within the target tissue causing a chemical reaction resulting in a healing response. This process is known as mechanotransduction. Essentially, mechanotransduction converts mechanical stimuli (pulses of acoustic waves) into a positive cellular healing response (Mittermayr et al., 2021).
How does focused shockwave treat bony injuries?
Focused shockwave has been proven to promote bone healing (Leal et al., 2015; Roche et al., 2020; Mittermayr et al., 2021). Bone healing occurs via the following pathways:
Osteoinduction
Focused shockwave has been shown to stimulate integrins. Integrins are transmembrane receptors (located on the cell membrane) and are responsible for binding the cell to the extracellular matrix. The extracellular matrix provides structure and support for all connective tissue including bone and so is an essential component of healthy tissue (Mittermayr et al., 2021).
Importantly the activation of integrins, via focused shockwave, has been shown to be effective at stimulating osteoblast activity (osteoblasts are cells which are responsible for laying down new bone tissue). Effective osteoblast activity is essential for bone healing (Leal et al., 2015; Mittermayr et al., 2021).
Research has also shown that focused shockwave stimulates the production of both transforming growth factor (TGF) and vascular endothelial growth factor (VEGF). These two specialist signalling proteins are responsible for stimulating many biological processes including the development of new blood vessels and bone marrow cells known as mesenchymal cells, which further develop into osteoblasts. Both these processes are essential for the development of new bone (Hoffman et al., 2008. Wang et al., 2002).
Periosteal stimulation
Focused shockwave is believed to stimulate the periosteum causing cells to migrate into the damaged area. This results in the development of a callus over the site of injury (Roche et al., 2020).
Neovascularisation
Normal bone tissue is highly vascular (receives a large amount of blood). To develop and sustain healthy bone it is essential that the blood supply is maintained. Focused shockwave has been shown to stimulate the development of new blood vessels in damaged bone, a process known as neovascularisation (Roche et al., 2020).
What does the research say about focused shockwave and delayed-union and non-union fractures?
Research supports the use of focused shockwave for treating both delayed and non-union fractures, reporting it to be a reliable and safe modality (Mittermayr et al., 2021) with a success rate as high as 85% (Schleusser et al., 2020).
Sound waves produced during the application of focused shockwave stimulate the cellular response at the fracture site, increasing the rate of fracture healing. Furthermore, research has shown focused shockwave to increase local blood supply and produce an effective hematoma (blood clot) at the site of the fracture (Li et al., 2021). The impressive outcomes attributed to focused shockwave were achieved without any complications being noted.
Bones successfully treated with focused shockwave have included the tibia, fibula, humerus, 5th metatarsal, and the scaphoid (Mittermayr et al., 2021).
Focused shockwave success is dependent on two factors, the size of the fracture gap and a good preservation of the blood supply. Fractures showing a gap of over 4.2 mm do not respond well to focused shockwave (Li et al., 2021). This is because the gap is too wide for natural healing to occur. Surgical intervention is required for treating patients with a gap size of over 4.2mm. Diagnostic ultrasound has been shown to be highly effective at measuring the fracture site gap as well as assessing for local blood flow and, therefore, can be used to assess the expected effectiveness of focused shockwave for this patient group (Schleusser et al., 2020).
Currently we are lacking in double-blind randomised controlled trials (the highest level of scientific research) to support the use of focused shockwave for treating delayed and non-union fractures, but the research we do have has shown very promising outcomes (Sansone et al., 2022).
What does the research say about focused shockwave and stress fractures?
The international society for medical shockwave treatments approves the use of focused shockwave for the treatment of stress fractures. There is a large volume of research supporting the use of focused shockwave for stimulating a healing response in bone injuries, and the basic science on how shockwave works supports its use for stress fractures. The evidence we have (albeit low quality i.e., case studies) shows promising results for stress fracture healing. However, to date, there are no high-level research articles available to confirm its efficacy.
Is focused shockwave painful?
Focused shockwave for treating bone conditions is painful but tolerable. might feel sore for a few days after receiving focused shockwave. It is advised that you limit physical activity until symptoms calm down.
Can I keep taking painkillers?
Focused shockwave is a pro-inflammatory treatment. Inflammation is an important part of the healing process. It sets the scene for healing to occur. Focused shockwave stimulates an inflammatory response within the target tissue. To allow healing to occur taking non-steroidal anti-inflammatories (NSAIDS) for the following 48 hours is not recommended. You can still take paracetamol if needed after focused shockwave.
Is focused shockwave safe?
Focused shockwave is very safe with very few side effects. There have been no reports of serious adverse effects following the use of focused shockwave either in bone, tendon, or men’s health conditions.
Are there any contraindications to focused shockwave?
Focused shockwave is not suitable for all. There are a few situations when focused shockwave cannot be used. These are:
- If you are pregnant.
- If you have a localised skin infection or the skin is cut or broken at the site of the fracture.
- If you have a blood clotting disorder or are taking blood thinning medication.
- If you have a pacemaker.
- If you have had a steroid injection in the last 6 weeks.
- If you are under the age of 18.
- Over an air-filled cavity such as the lungs.
What are the advantages of focused shockwave over other conservative treatments?
Conservative options for treating bone conditions are predominantly passive. Treatment is designed to allow the bone time to heal whilst limiting further stress (, for example, offloading the bone by limiting weight-bearing and using a brace). This is incredibly important and must still be adhered to when undertaking a course of focused shockwave. Focused shockwave, however, is a proactive treatment which actively stimulates the bone to remodel and heal. Stimulating healing during recovery allows for fast and effective outcomes to be achieved.
How is focused shockwave delivered?
Focused shockwave is delivered directly to the injured bone. A small amount of water-based gel is applied to the skin prior to treatment. This is to allow an easy passage for the soundwaves to pass from the shockwave machine into the body. The shockwaves are directed to the bone through a soft, cone-shaped handset which is placed on top of the gel, over the injury.
A series of pulses is then delivered (on average 2000 to 3000 pulses per treatment session). The machine makes a loud ticking noise as it delivers the shockwave dose. The speed and power of the shockwaves can be adjusted by the clinician, depending on patient tolerance.
You should feel discomfort during the duration of the treatment, but this should not be intolerable. It is important that you communicate with the clinician during treatment to ensure the correct dosage is given.
How long does focused shockwave take?
Focused shockwave takes between five to seven minutes to complete. Afterwards your clinician will provide you with information on what to expect following your treatment
How many sessions of focused shockwave do I need?
A course of focused shockwave consists of between four to eight sessions spaced one week apart. A course of focused shockwave consists of between three to eight sessions, depending on the severity and chronicity of the injury, as well as how you respond to the initial sessions. Your clinician will be able to advise you on the expected number of sessions you will require after you have had your first session.
What can I do to help maximise my outcomes?
It is vitally important to continue with all your other conservative treatments whilst undertaking focused shockwave. This might mean continuing to wear your brace or to continue with your exercise program. You will be directed on what to do by your clinician during your session.
If you have any questions, please do not hesitate to contact the clinic at info@complete-physio.co.uk or on 020 7482 3875
References:
Hofmann, A., Ritz, U., Hessmann, M.H., Alini, M., Rommens, P.M. and Rompe, J.D., 2008. Extracorporeal shock wave-mediated changes in proliferation, differentiation, and gene expression of human osteoblasts. Journal of Trauma and Acute Care Surgery, 65(6), pp.1402-1410.
Leal, C., D’Agostino, C., Garcia, S.G. and Fernandez, A., 2015. Current concepts of shockwave therapy in stress fractures. International Journal of Surgery, 24, pp.195-200.
Li, A., Wang, R., Yu, S., Huang, J., Jiang, L. & Li, X. 2021, Analysis of Related Factors Influencing the Efficacy of Extracorporeal Shockwave in the Treatment of Fracture Nonunion: A Prospective Study in Shanghai, China, Research Square Platform LLC.
Mittermayr, R., Haffner, N., Feichtinger, X. & Schaden, W. 2021a, The role of shockwaves in the enhancement of bone repair – from basic principles to clinical application, Elsevier BV.
Roche, M., Abrams, G. & Fredericson, M. 2020, “Systemic Treatment Modalities for Stress Fractures” in Stress Fractures in Athletes Springer International Publishing, Cham, pp. 141-149.
Sansone, V., Ravier, D., Pascale, V., Applefield, R., Del Fabbro, M. & Martinelli, N. 2022, Extracorporeal Shockwave Therapy in the Treatment of Nonunion in Long Bones: A Systematic Review and Meta-Analysis, MDPI AG.
Schleusser, S., Song, J., Stang, F.H., Mailaender, P., Kraemer, R. & Kisch, T. 2020, Blood Flow in the Scaphoid Is Improved by Focused Extracorporeal Shock Wave Therapy, Ovid Technologies (Wolters Kluwer Health).
Sheen, J.R. and Garla, V.V., 2021. Fracture healing overview. In StatPearls [Internet]. StatPearls Publishing.
Wang, F.S., Yang, K.D., Chen, R.F., Wang, C.J. and Sheen-Chen, S.M., 2002. Extracorporeal shock wave promotes growth and differentiation of bone-marrow stromal cells towards osteoprogenitors associated with induction of TGF-β1. The Journal of Bone and Joint Surgery. British volume, 84(3), pp.457-461.
Don’t let pain hold you back, book now!