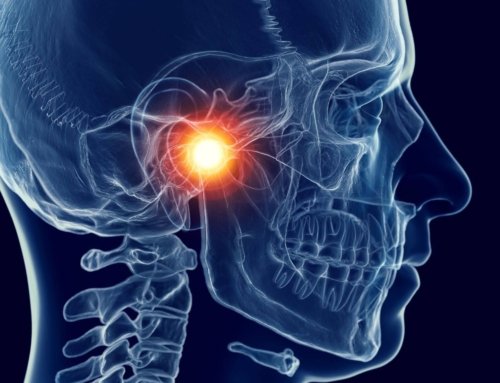
What is Sciatica?
Sciatica is a symptom caused by pressure on the lumbar or sacral nerve roots; while the pain is felt down the leg, along the sciatic nerve, the source of the compression is located at the spine.
Sciatica is most commonly caused from a herniated or ‘slipped’ disk, that pinches or puts pressure on the nerve root as it exits the spine; however, there are numerous causes of sciatic pain which will be highlighted in this article.
Most people with sciatica respond incredibly well to physiotherapy and conservative treatments. At Complete Physio we see hundreds of patients with Sciatica, and have an expert team who can ensure you make a full and speedy recovery.
Anatomy of the Sciatic Nerve
The sciatic nerve is a large nerve extending from your lower back down the back of each leg.
It originates from the bottom five spinal vertebrae – L4, L5, S1, S2 and S3. It is the longest, thickest nerve in the body (a finger width in diameter).
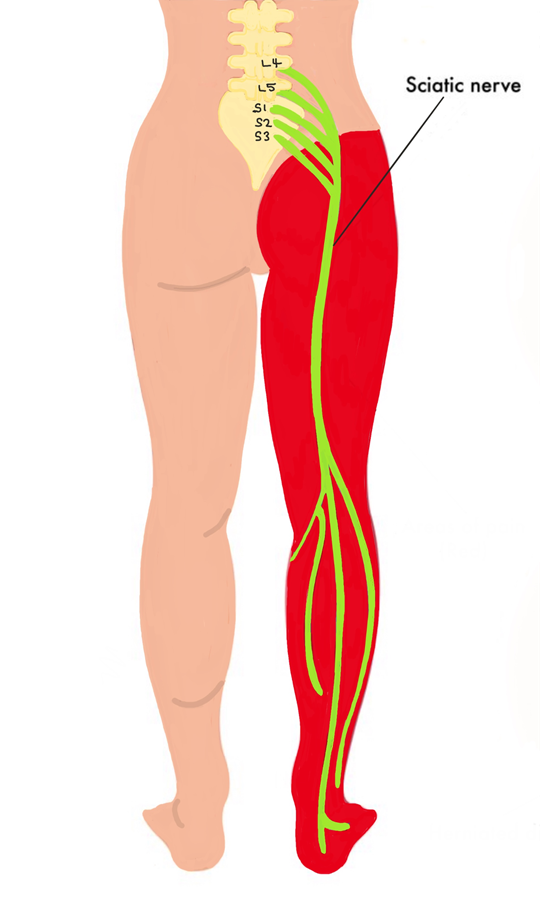
You have a sciatic nerve on each side of your body that runs through your hips, buttocks and down the back of your leg, ending just below the knee. The sciatic nerve then branches into other nerves, which continue down your leg and into your foot and toes.
What Causes Sciatica?
‘Sciatica’ is technically not a diagnosis, but rather the symptom of a problem involving the sciatic nerve. The term ‘sciatica’ is used to describe any pain that originates in the lower back and radiates down the leg. ‘Sciatica’ can exist with or without lower back pain.
Anything that irritates or compresses the sciatic nerve can cause sciatic pain. However, true nerve injury to the sciatic nerve is actually quite rare.
As mentioned previously, the most common cause of sciatica is a herniated disc. The disc bulges outwards and irritates or compresses the nerve root, and causes pain and symptoms that radiate along the line of the sciatic nerve. It is not uncommon that you have a herniated disc and no lower back pain, but do experience leg pain.
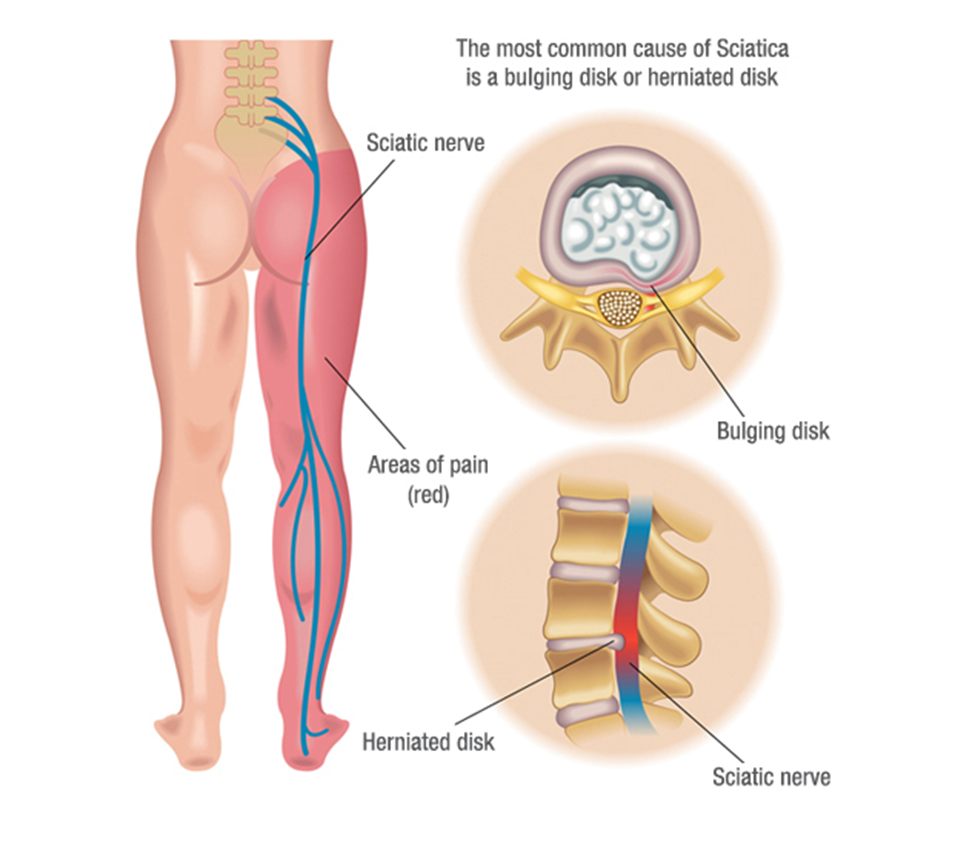
Other causes of sciatica are:
- Spine Degeneration – This can be a wear and tear of the discs or osteoarthritic changes in the bony vertebrae. Either can cause irritation or compress the sciatic nerve.
- Spinal Stenosis – is the abnormal narrowing of the spinal canal due to bone spurs (extra bone growth) which reduces the available space for the spinal cord and nerves. This typically affects people aged 60 or over.
- Spondylolisthesis – when one vertebrae slips out of line slightly with the one above or below, which narrows the opening where the nerve root exits the spine.
- Piriformis Syndrome – This is very rare. The sciatic nerve may pass through a muscle in the buttocks called the piriformis. This muscle can sometimes tighten and spasm which compresses and constricts the sciatic nerve, producing symptoms. Deep Gluteal Syndrome is a broader term for this as there are other deep muscles in the buttocks that can ‘entrap’ the sciatic nerve, depending on its course.
Much less common sources include:
- Tumours in the lumbar spine or pelvis
- Direct trauma to the spine or sciatic nerve such as a knife wound
- Pregnancy
You’re most likely to get sciatica between the ages of 30 to 50 years old, but it can occur at any age depending on the underlying pathology.
Nerves are hypersensitive, and even a mild irritation can cause significant pain and inflammation. While they are easily aggravated, they can be quite tricky to settle down, and therefore it is important that you seek help from an experienced professional in order to ensure you are treated quickly and appropriately.
What are the symptoms of Sciatica?
Sciatic pain can range from mild to severe; for some people it can be an infrequent irritation, while for others it can be severely debilitating. Classic sciatic pain starts in the low back and buttocks, it usually only affects one side of the body, extending all the way through the back of your thigh and down your leg, and is often described as a burning or shooting pain. Depending on the exact cause and location of where the sciatic nerve is affected, the pain may also extend to the foot or toes. It can also cause symptoms of muscle weakness, numbness, and a tingling, pins-and-needles sensation in your leg, foot and toes.
Sitting and bending often aggravates the symptoms, and walking and gentle movement will usually give some relief. Often it is the leg pain and symptoms that are worse than the back pain.
Common Symptoms of Sciatica
- Moderate to severe pain in lower back, buttock and down your leg.
- Burning or shooting pain in the leg
- A sensation of weakness in your leg or foot.
- Pain that worsens with sitting (especially driving) or bending
- “Pins and needles” or a feeling of numbness in your legs, toes or feet.
IMPORTANT: You should be aware that if you are suffering symptoms of extreme bilateral leg weakness (both legs), numbness in the groin or genital area, or loss of bladder or bowel function, you should seek medical help immediately, as these can be symptoms of a more serious condition called cauda equina syndrome, which needs emergency treatment and you should attend A & E.
How is Sciatica diagnosed?
It is important that you get a quick and accurate diagnosis in order to ensure that you are started on the correct treatment pathway. In most cases, Complete Physio are able to offer urgent, same day or next day appointments if needed.
Sciatica is a clinical diagnosis and can be accurately diagnosed by an experienced physiotherapist.
Your physiotherapist will listen and take a full account of your injury, asking questions about your symptoms, your general health, your past medical history, and what your normal daily activities and sports are.
They will then complete a thorough physical examination and a series of clinical tests to help develop a diagnosis. Depending on the severity of your symptoms your spinal physical assessment will include assessing:
- Range of movement of your spine and pelvis
- Muscle strength of your core and lower leg muscles
- Sensory and motor impairment
- Reflexes
- Spinal posture
- Pelvic and core stability
- Gently, but skillfully palpating the spine and the surrounding structures and tissues
- Special tests – straight leg raise and slump test (see below), which may provoke your pain
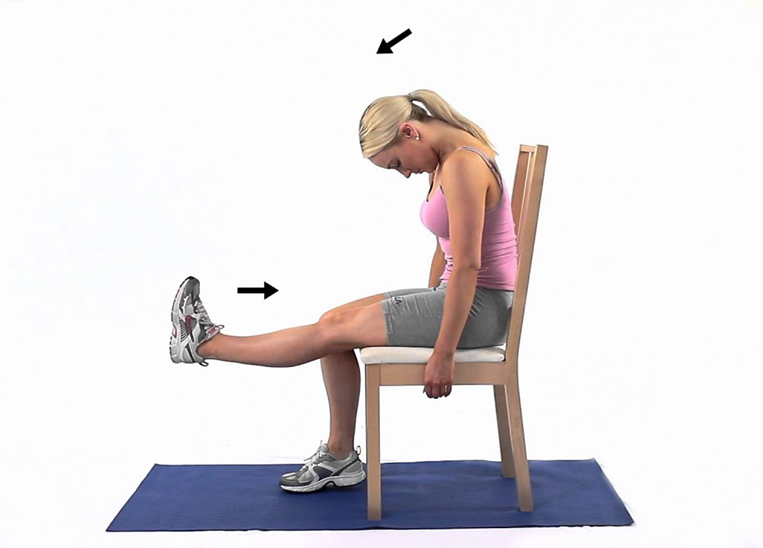
Image: slump test
These assessments combined are usually all that is required to diagnose your condition, however, while the diagnosis of sciatica is reasonably straightforward, the primary cause of your sciatica may require further investigations to eliminate or confirm its origin. Where symptoms are severe and not settling with treatment, or if the underlying diagnosis is unclear, your physiotherapist can refer you for additional diagnostic tests such as an MRI.
What imaging do you need if you have been diagnosed with sciatica?
X-RAY
X-rays are only able to show bony injuries and not soft tissue or nerve damage, therefore they have limited use when diagnosing sciatica. However if a spinal fracture is suspected, or other bony pathologies, then an x-ray may be useful.
MRI
An MRI scan consists of a series of pictures which create a highly detailed, 3D image, allowing for visualisation of your injury, and enabling an accurate diagnosis.
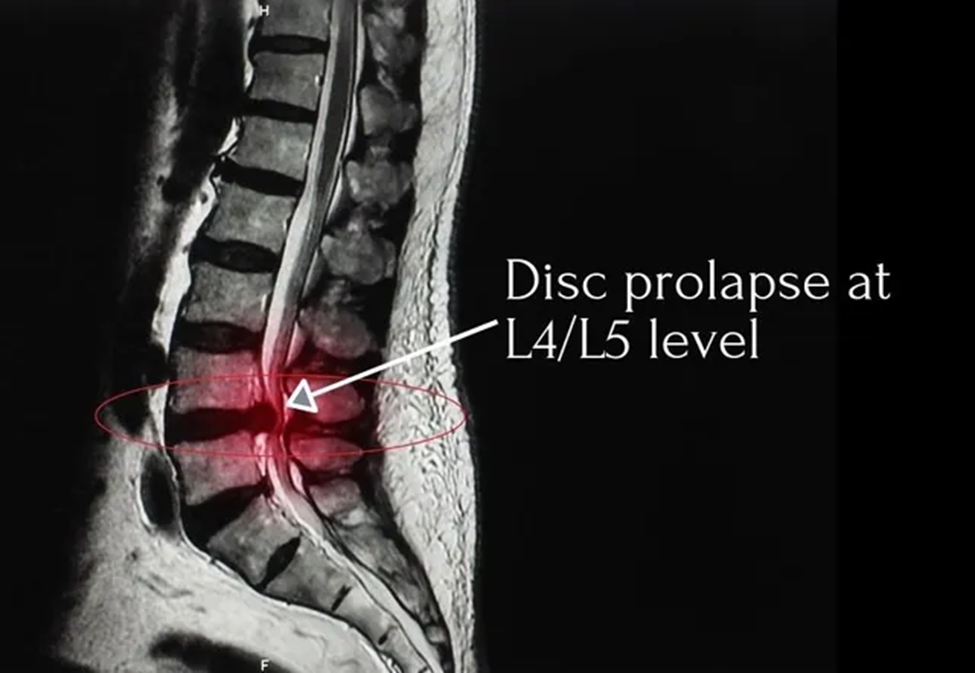
Occasionally an MRI scan can be needed if your clinician suspects a more serious root cause to your sciatica, such as a tumour or if a person has suffered from an injury or trauma.
How do we treat Sciatica?
The good news is that the majority of cases of sciatica resolve well with conservative management within a few weeks or months. The goal of treatment is to reduce your symptoms, restore function, and prevent re-injury.
Physiotherapy
Physiotherapy is an essential part of conservative management for sciatica. There are a number of treatment options that your physiotherapist will discuss with you, and together you will work out a treatment plan based on the symptoms, and your own, personal goals. Your treatment plan will likely combine pain relief techniques, stretching, strengthening, acupuncture, core conditioning and posture/movement reeducation.
Pain Management
Initially your physiotherapy will focus on treatments that help settle your pain. This may include using heat or ice, soft tissue massage, and if appropriate acupuncture.
Your physiotherapist will also give you advice on rest and activity modification, to reduce further flare ups while your pain subsides. During this phase it is often useful to take a short course of medication to help manage your symptoms.
Medication
Over-the-counter nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen or naproxen, can help to reduce swelling and inflammation of the nerves. If you are experiencing muscle spasms, a muscle relaxant may be prescribed, and if the pain is severe, a painkiller can also be prescribed that can be taken with the NSAID or muscle relaxant. You must always seek professional advice from your GP, pharmacist or qualified prescriber before taking any medication.
Soft Tissue Massage
Massage is incredibly useful to help reduce tension and muscle spasms, and it also has relaxation benefits.
Acupuncture or Dry Needling
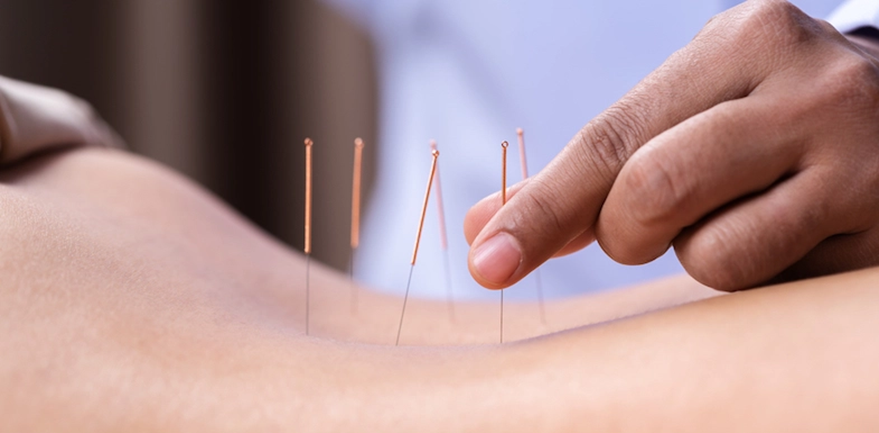
There is good quality evidence to show that acupuncture is an effective treatment option for sciatic. Acupuncture has been proven to help with pain and muscle spasm, improving blood circulation, regulating the nervous system, and releasing neurotransmitters to reduce pain.
Restoring Movement and Strength
Stretches
You will be given movement exercises to improve joint range of your lumbar spine, hips and pelvis, as well as muscle stretches to help lengthen tight muscles. It is important to be aware sometimes stretches can actually increase your pain if you have sciatica. It is essential that any exercise is prescribed by a physiotherapist with vast experience in treating sciatica
Strength and Endurance
You will need to work on your postural and core strength. Your physiotherapist will commence you on a strengthening programme that specifically focuses on back stability, and targets the deep postural muscles that dynamically control and stabilise your lower back and pelvis.
Your physiotherapist may also suggest that you commence a course of Pilates and rehabilitation, which is a highly effective way of managing mechanical low back pain. At Complete Physio we offer a variety of treatments for sciatica to reduce your pain and get you moving in the right direction.

Restoring Full Function
Functional and Posture Re-education
Your physiotherapist will assess the way you move and do functional tasks. Depending on your occupation, or chosen sport or activities, your physiotherapist will tailor your rehabilitation to work on specific actions or high level functional movements, to allow you to return to your desired activities safely.
They will work on your sitting posture and movement patterns, and correct any abnormalities.
Sciatica can sometimes return; the main reason for recurrence is often due to insufficient or incomplete rehabilitation. Fine-tuning your back mobility and building up your core control and strength is very important, as well as learning self-management techniques. Your Physiotherapist will work closely with you to ensure you have a long term plan, and a good understanding of your condition, so that you feel confident to continue your exercises programme independently, ensuring that your symptoms do not return.
Spinal Injections for Sciatica
If your symptoms are not settling with physiotherapy alone, or if your pain is so severe that it is preventing you from fully engaging in your rehabilitation programme, spinal injections may be an appropriate next step.
At Complete Physio, spinal injections are delivered through our specialist service, Complete Injections, led by Dr Matteo Bernardotto, a highly experienced consultant in musculoskeletal and spinal injections. For sciatica, the most commonly recommended procedure is a selective nerve root injection.
Nerve root injections involve the precise delivery of a local anaesthetic and corticosteroid medication around the irritated spinal nerve root under image guidance. This helps to reduce inflammation, swelling, and pain at the source of your symptoms, often resulting in significant relief of leg pain.
It is important to note that spinal injections are not a standalone treatment. Their primary role is to reduce pain to a level that allows you to fully engage in and benefit from a structured physiotherapy programme. In some cases, nerve root injections are also used diagnostically, helping to confirm which nerve is responsible for your symptoms.
Your physiotherapist will only recommend an injection if it is clinically appropriate and will work closely with Dr Bernardotto and the Complete Injections team to ensure your care is joined-up, evidence-based, and focused on long-term recovery.
Surgery for Sciatica
Typically, spinal surgery for sciatica is not advised until all other conservative treatment options have failed to provide relief.
There are a few instances when surgery would be considered as the first point of call:
- Cauda equina syndrome – This requires immediate surgical intervention.
- Bilateral sciatica – Sciatica that affects both legs can be brought on by central spinal stenosis, severe single-level herniation, or multiple-level disc herniation.
- Tumours
- Severe lumbar spine fractures
We work with some of the best and most experienced surgeons in the country, so again, if an onward referral to a spinal surgeon is needed, we will ensure that you are provided with the best care possible. Following surgery we will continue to support your post op recovery and rehabilitation every step of the way.
If you would like to book an appointment or speak to one of our expert physiotherapists please call 020 4600 4007 or email info@complete-physio.co.uk.
Don’t let pain hold you back, book now!