Shockwave therapy for proximal hamstring tendinopathy
1. What is proximal hamstring tendinopathy?
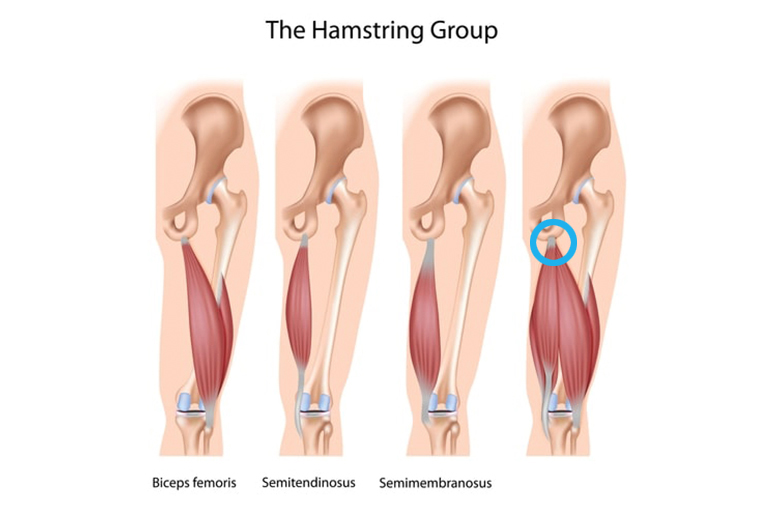
The hamstring complex is made of three muscles (see below);
- Biceps femoris
- Semitendinosus
- Semimembranosus
Proximal hamstring tendinopathy (circled in blue below) is where the tendons attach to the ischial tuberosity (sitting bone) and was first described as “hamstring syndrome” by Puranen and Orava (1988).
Proximal hamstring tendinopathy is also known as high hamstring tendinopathy, or hamstring origin tendinopathy.
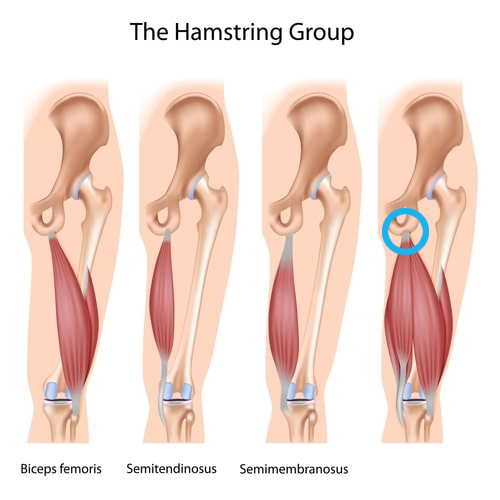
Proximal hamstring tendinopathy is not typically associated with a single traumatic event, but instead represents a chronic degenerative process produced by mechanical overload of the muscle/tendon and repetitive stretch (Chu SK & Rho ME, 2017)
Patients with proximal hamstring tendinopathy often have pain around their buttock crease which refers down the leg, most notable when participating in running activities, where hip flexion and knee extension elicit symptoms (Chu SK & Rho ME, 2017)

Occasionally, symptoms of sciatic nerve irritation may also develop along with their tendinopathy. (Degen, 2019)
2. What causes proximal hamstring tendinopathy?
The exact cause is often unknown, but there are certain features and sports such as running, which can provoke the condition.
The hamstring complex spans both the hip and knee therefore the hamstring tendons are at a higher risk of injury due to the possibility for rapid muscle lengthening with combined hip flexion and knee extension noted during the swing phase of sprinting or running (Ahamd et al., 2013, Cohen, 2007, Chu SK & Rho ME, 2016)
Other risks factors for proximal hamstring tendinopathy are;
- Poor lumbopelvic stability (Chu SK & Rho ME, 2017)
- Weak hamstrings (Fredericson M et al., 2005)
- Prolonged sitting or driving in a car [Cacchio A et., 2011).
- Over stride pattern whilst running (see image above)
3. How do we treat proximal hamstring tendinopathy?
Most proximal hamstring tendinopathy pain resolves with a course of physiotherapy.
It is however common for tendinopathy problems to take 3 months to resolve if the condition is chronic (if you have had it greater than 12 weeks).
Research shows that treatment should involve heavy loading/strengthening for the glutes, hamstring muscles and the proximal hamstring tendon.
If you are not improving with rehabilitation and physiotherapy, shockwave therapy or an ultrasound guided injection may be an suggested management strategy to your treatment.

4. Is shockwave therapy effective for proximal hamstring tendinopathy?
There is evidence to suggest shockwave therapy is advantageous in managing proximal hamstring tendinopathy. Cacchio et al (2011) conducted a study on 40 professional athletes with proximal hamstring tendinopathy treated with conservative therapy or shockwave therapy and found patients in the shockwave group had improved pain at 12 months follow up.
Cacchio et al (2011) concluded that shockwave therapy was a safe and effective treatment for proximal hamstring tendinopathy.
At Complete we treat a large number of clients with proximal hamstring tendinopathy and the combination of shockwave therapy and rehabilitation exercises has improved clinical results.
5. How many sessions and how often do you need shockwave therapy for proximal hamstring tendinopathy?
At Complete we are guided by the latest evidence-based research for our shockwave protocols (see below). We advise a minimum of three shockwave sessions roughly one week apart, however other patients may require additional sessions, but this will depend patient’s and the hamstring response.
Recommendation:
2500 impulses at 4.0 bars (energy flux density 0.18mJ/mm2) at 10Hz for four sessions at weekly intervals (Cacchio et al, 2011; Korakakis et al,
6. How long does it take to recover from proximal hamstring tendinopathy?
This varies from person to person depending on the type and severity of the tendinopathy. Some patients feel an instant decrease in their pain following the first shockwave session, while for others it may take longer.
7. Should you have an ultrasound scan or an MRI before having shockwave therapy?
The use of an ultrasound scan can be valuable to further assess your proximal hamstring tendon to confirm your diagnosis if your therapist is unsure of your diagnosis. At Complete we undertake an ultrasound scan at no extra cost and you do not need a GP referral. If you require a diagnostic ultrasound scan, please inform the reception team when booking.
An ultrasound scan will answer the following questions:
- Which hamstring tendons are involved?
- Is there any ischial bursitis?
- What is the severity of tendinopathy?
- Is there a significant tear in the tendon
If you would like to book an appointment or would like more information before booking, please call 020 7482 3875 or email info@complete-physio.co.uk
References: