Ultrasound Guided Injections – So where’s the Point?
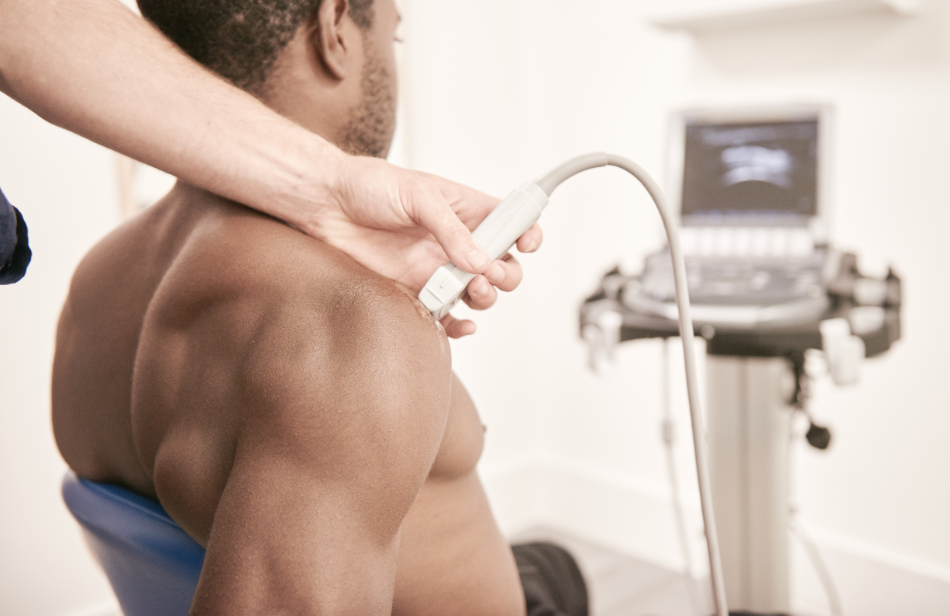
At Complete Physio we perform all of our injections under ultrasound guidance and have done so for many years. Ultrasound guided injections are performed by clinicians who are specialists in musculoskeletal sonography, as well as highly trained and experienced physiotherapists, which enables the injection to be performed with absolute precision.
We believe that all injections should be performed under ultrasound guidance to achieve the best possible outcomes, to reduce and minimise the risks of potential harm, so the result of the injection can be used to assist with clinical reasoning.
Trials of ultrasound guided injections
There are a growing number of trials in recent years which show evidence that ultrasound guided injections are more effective for treating a range of musculoskeletal disorders than when an injection is performed ‘blind’ or with ‘surface marking’ only.
There is also strong evidence that when a joint or a structure needs aspiration (draining of fluid or swelling), this can be done far more effectively and efficiently with ultrasound guidance.
However, this is by no means the only reason why we choose to perform our injections or aspirations in this way.
Firstly, and probably most importantly, because our physiotherapists who perform ultrasound guided injections are also fully trained musculoskeletal sonographers, they can fully evaluate the area prior to the injection to confirm the diagnosis and to ensure there is no reason why an injection might be the wrong treatment or be unsafe.
It also allows the clinician to ensure that there are no nerves or vessels in the path of the needle on its way to the target structure, which could potentially cause risk of nerve and/or vascular damage.
Reduced risk when using Ultrasound guided injections
Additionally, when injecting steroid, there is a risk of depigmentation and fat atrophy to the area. It has been shown that by using ultrasound guidance, where the needle tip can be placed more accurately, the risk of this is reduced.
There have also been studies, including a Cochrane Library review, that conclude the overall risk of side effects are reduced when having an ultrasound guided injection (Bloom 2012).
Furthermore, because we can be sure of the accuracy of the injection, the need for further injections can be reduced. If the patient does not get the desired outcome in the first instance, then we know that other modes of treatment may need to be considered.
This decision can be made more reliably when an injection is performed under ultrasound guidance.
Increasing range of ultrasound guided injections
We are also using an increasing range of injection therapies, such as hyaluronic acid (a substance which may act to reduce pain in osteoarthritic joints and help to facilitate the body’s natural nourishment and lubrication to joint surfaces, also can sometimes be used around tendons to reduce pain), which certainly needs to be injected under ultrasound guidance, not least because it is expensive, but also because it would unlikely give any benefit if it was not placed accurately into the joint or around the structure that was to be targeted.
We also offer other specialist injection techniques, such as barbotage (a technique whereby small calcific deposits within tendons can be broken down and drained or aspirated) and high volume injections which especially require ultrasound guidance in order for them to be performed effectively.
Ultrasound guided injections by qualified personnel
All our injecting physiotherapists are also qualified as independent prescribers.
This means they have undertaken vigorous training to be able to select and prescribe the best drug for your treatment.
It also means they have additional skills in being able to assess you for potential side effects and risks, and have a deeper understanding of the drugs that are being used so that they can select the best medication for your condition.
For your convenience, no referral is required from your GP or consultant – patients are able to self refer or be referred by any healthcare professional.
Ultrasound guided injections summary
In summary: At Complete Physio we firmly believe that all injections should be performed under ultrasound guidance by expert clinicians, with many years of experience in order that we can offer the safest, most effective treatment for our patients.
Written by David Baker
Chartered Physiotherapist (HPC & CSP Member)
Clinical Director
Extended Scope Practitioner and Independent Prescriber
Associated Professional member of the Society of Radiographers - PG Cert MSK Sonographer
Visiting Lecturer
Chairman of Association for Chartered Physiotherapists with an interest in Orthopaedic Medicine and Injection Therapy
Follow on @davebakerphysio
References
Arnold, J., P. Anthonioz, and J. P. Marchand. "Depigmenting action of corticosteroids." Dermatology 151.5 (1975): 274-280.
Balint, Peter V., et al. "Ultrasound guided versus conventional joint and soft tissue fluid aspiration in rheumatology practice: a pilot study." The Journal of rheumatology 29.10 (2002): 2209-2213.
Berkoff, David J., Larry E. Miller, and Jon E. Block. "Clinical utility of ultrasound guidance for intra-articular knee injections: a review." Clinical interventions in aging 7 (2012): 89.
Bloom, Jason E., et al. "Image‐guided versus blind glucocorticoid injection for shoulder pain." The Cochrane Library (2012).
Brinks, Aaltien, et al. "Adverse effects of extra-articular corticosteroid injections: a systematic review." BMC musculoskeletal disorders 11.1 (2010): 206.
Bum Park, Yong, et al. "Accuracy of blind versus ultrasound‐guided suprapatellar bursal injection." Journal of Clinical Ultrasound 40.1 (2012): 20-25.
Canturk, F., et al. "Cutaneous linear atrophy following intralesional corticosteroid injection in the treatment of tendonitis." CUTIS-NEW YORK- 73.3 (2004): 197-198.
Chen, Max JL, et al. "Ultrasound-guided shoulder injections in the treatment of subacromial bursitis." American journal of physical medicine & rehabilitation 85.1 (2006): 31-35.
Dean, Benjamin John Floyd, et al. "The risks and benefits of glucocorticoid treatment for tendinopathy: A systematic review of the effects of local glucocorticoid on tendon." Seminars in arthritis and rheumatism. Vol. 43. No. 4. WB Saunders, 2014.
Habib, George S. "Systemic effects of intra-articular corticosteroids." Clinical rheumatology 28.7 (2009): 749-756.
Habib, George S., Walid Saliba, and Munir Nashashibi. "Local effects of intra-articular corticosteroids." Clinical rheumatology 29.4 (2010): 347-356.
Jeyapalan, Kanagaratnam, and Surabhi Choudhary. "Ultrasound-guided injection of triamcinolone and bupivacaine in the management of de Quervain′ s disease." Skeletal radiology 38.11 (2009): 1099-1103.
Kumar, Naresh, and Raymond J. Newman. "Complications of intra-and peri-articular steroid injections." British journal of general practice 49.443 (1999): 465-466.
Lavelle, William, Elizabeth Demers Lavelle, and Lori Lavelle. "Intra-articular injections." Anesthesiology clinics 25.4 (2007): 853-862.
Lee, Hong-Jae, et al. "Randomized controlled trial for efficacy of intra-articular injection for adhesive capsulitis: ultrasonography-guided versus blind technique." Archives of physical medicine and rehabilitation 90.12 (2009): 1997-2002.
McNally, Eugene G., and Shilpa Shetty. "Plantar fascia: imaging diagnosis and guided treatment." Seminars in musculoskeletal radiology. Vol. 14. No. 3. 2010.
Nichols, Andrew W. "Complications associated with the use of corticosteroids in the treatment of athletic injuries." Clinical Journal of Sport Medicine 15.5 (2005): E370.
Papadopoulos, Patricia J., and Jess D. Edison. "Soft tissue atrophy after corticosteroid injection." Cleveland Clinic journal of medicine 76.6 (2009): 373-374.
Rutten, Matthieu JCM, et al. "Injection of the subacromial-subdeltoid bursa: blind or ultrasound-guided?." Acta orthopaedica 78.2 (2007): 254-257.
Sinatra R S, Jahr J S and Watkins-Pitchford J M (2011) The Essence of Analgesia and analgesics. Cambridge University Press.
Spinner, David A., Jonathan S. Kirschner, and Joseph E. Herrera, eds. Atlas of ultrasound guided musculoskeletal injections. Springer New York, 2014.
Tatli, Yusuf Ziya, and Sameer Kapasi. "The real risks of steroid injection for plantar fasciitis, with a review of conservative therapies." Current reviews in musculoskeletal medicine 2.1 (2009): 3-9.
Yucel, Istemi, et al. "Comparison of ultrasound-, palpation-, and scintigraphy-guided steroid injections in the treatment of plantar fasciitis." Archives of orthopaedic and trauma surgery 129.5 (2009): 695-701.