A Longer-Lasting Option for Persistent Knee Pain
Knee osteoarthritis (OA) is one of the most common causes of long-term joint pain we see at Complete Physio.
For many patients, symptoms fluctuate, there are manageable days, and then there are painful flare-ups that significantly impact walking, stairs, exercise and quality of life.
In recent years, Arthrosamid® has emerged as a newer injectable treatment option for knee osteoarthritis.
While it may be described as a “new kid on the block,” the science behind it has been around for over 20 years.
Key Takeaways from This Article
- Arthrosamid is a non-biodegradable hydrogel injection designed to reduce inflammatory flare-ups in knee osteoarthritis.
- It works differently from steroids and hyaluronic acid; integrating into the synovial lining rather than coating cartilage.
- It does not cure osteoarthritis, but may significantly reduce pain and improve function for up to 2-3 years in some patients.
- Patient selection matters – earlier-stage symptomatic OA tends to respond better than advanced end-stage disease.
- It sits between physiotherapy and surgery in the treatment pathway and can delay the need for knee replacement in some individuals.
- Best outcomes occur when combined with structured physiotherapy, strength training and load management – not as a standalone solution.
Understanding Knee Osteoarthritis
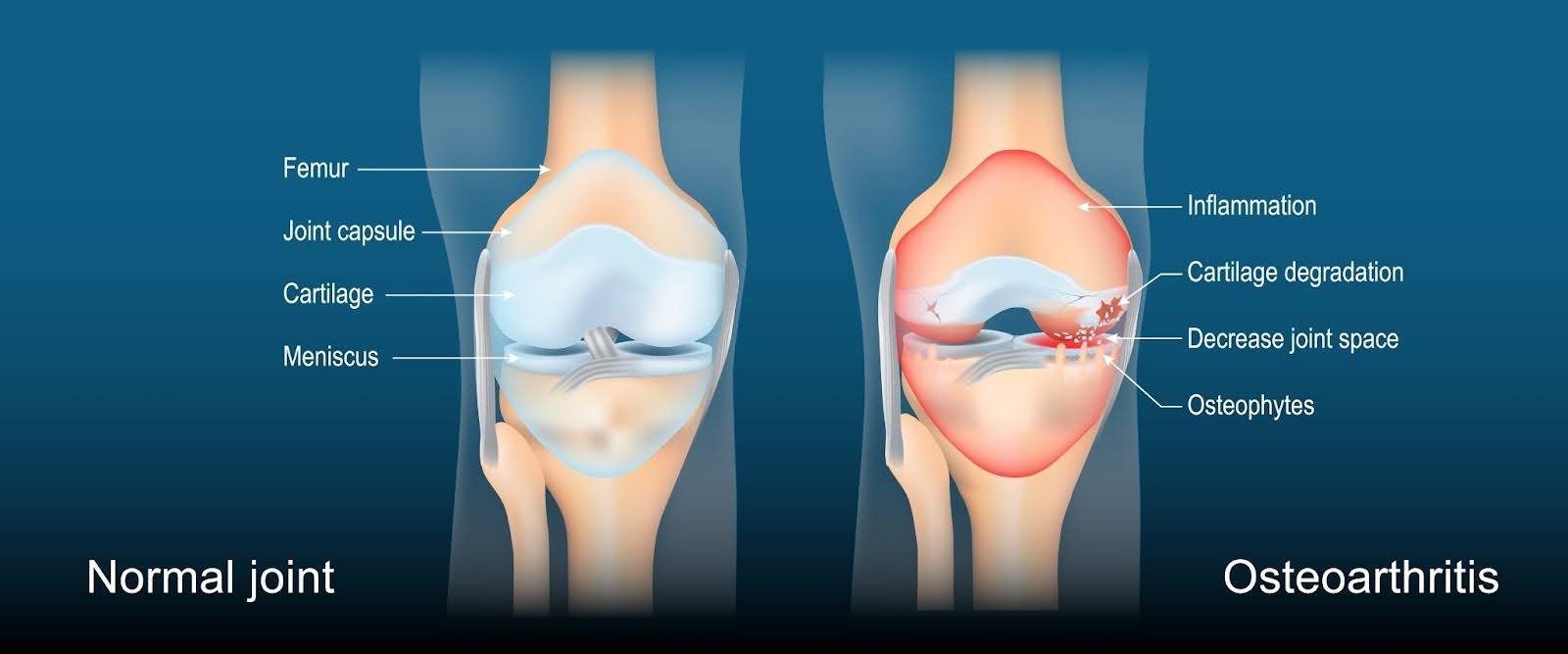
Knee osteoarthritis is a degenerative joint condition affecting the cartilage, the smooth, shock-absorbing surface that covers the ends of the bones.
Common symptoms include:
- Pain with walking, stairs or prolonged standing
- Stiffness, particularly in the morning or after rest
- Swelling or episodes of inflammation
- A feeling of grinding, clicking or instability
- Flare-ups triggered by twisting, overuse or minor injury
Importantly, people with knee OA do not usually experience constant severe pain. Instead, they often describe a “grumpy knee” that periodically flares up.
What Causes Flare-Ups?
Inside every joint is a capsule lined by a tissue called the synovium.
This inner lining produces joint fluid (synovial fluid) and helps lubricate the joint and regulate inflammation. In osteoarthritis, the synovium can become irritated and inflamed; a process known as synovitis.
The Synovial Pain Cycle (Synovitis)
In knee osteoarthritis, the synovial pain cycle begins when joint cartilage breakdown and mechanical stress irritate the synovial lining.
This irritation triggers low-grade inflammation within the joint, increasing the production of inflammatory mediators and excess synovial fluid.
The inflamed synovium becomes more sensitive and reactive, which amplifies pain signals.
Pain then leads to reduced movement and muscle inhibition, particularly in the quadriceps, causing muscle weakness and poorer load distribution through the knee.
That altered mechanics further aggravates the synovium, fuelling ongoing inflammation and creating a self-perpetuating cycle of pain, swelling, stiffness and reduced function.

These inflammatory flare-ups are often responsible for the sharp increases in pain that patients experience.
Repeated inflammation can also accelerate joint degeneration over time.
What Is Arthrosamid®?
Click to watch a video explaining Arthrosamid®
Arthrosamid is an injectable treatment composed of a non-biodegradable polyacrylamide hydrogel. In simple terms, it is a thick, highly viscous gel that is injected into the knee joint.
Unlike some traditional injections, Arthrosamid does not work by coating cartilage or temporarily suppressing inflammation. Instead, it works directly on the lining of the joint capsule – the synovium.
It is typically considered for individuals who have persistent symptoms despite good rehabilitation and shorter-acting injections, but who are not yet ready for surgery.
How Does Arthrosamid® Work?
Arthrosamid® works in two key ways:
1. It Acts as a Protective Barrier
Once injected, the hydrogel integrates into the synovial lining. It forms a physical barrier that helps block inflammatory signals from triggering synovial flare-ups.
Think of it as a “fire blanket” for inflammation, reducing the synovium’s ability to become excessively reactive.
2. It Integrates Into the Synovium
Over time, the synovial tissue grows around the hydrogel, embedding it within the lining of the joint. This integration creates a longer-term spacing effect between inflammatory cells, making it harder for them to “activate” collectively.
How Is It Different From Other Injections?
All joint injections have their place, and can be beneficial at different stages of knee OA. Here is a breakdown of each, with some pro’s and cons.
It’s important to remember that there is no ‘one size fits all’ and patient selection for each of these treatments is really important, to ensure the most effective treatment is used.
Your physiotherapist will discuss all your options before making an informed, joint decision on your treatment plan.
Corticosteroid Injections
Corticosteroid injections are a well-established and evidence-based treatment for knee osteoarthritis.
They work by reducing inflammation within the joint, often providing rapid pain relief.
For many patients, this can be particularly helpful during a flare-up, allowing them to move more comfortably and re-engage with physiotherapy and strengthening work.
While the effects typically last weeks to a few months rather than years, they can play an important role in managing symptoms at key stages of the condition.
When used appropriately and not too frequently, steroid injections remain a valuable and effective option within the broader treatment pathway for knee OA.
Key Benefits
- Rapid reduction in joint inflammation – often provides pain relief within a few days
- Particularly effective for inflammatory flare-ups
- Can improve mobility quickly, allowing return to physiotherapy and strengthening
- Minimally invasive, performed in clinic
- Cost-effective compared to some newer injection options
- Strong clinical track record with decades of use
Potential Limitations
- Pain relief is typically temporary (weeks to a few months)
- Effects can vary between individuals
- Repeated frequent injections may negatively affect joint cartilage
- Will not address underlying joint mechanics and muscle imbalances without rehabilitation alongside it
Hyaluronic Acid (HA) Injections
Hyaluronic acid (HA) injections are designed to supplement the natural joint fluid within the knee.
As mentioned, in osteoarthritis, the quality and concentration of hyaluronic acid in the synovial fluid often reduces, affecting lubrication and shock absorption. By restoring some of these properties, HA injections can help improve joint glide, reduce stiffness, and ease pain.
They don’t act as quickly as steroid injections, but for some patients they provide steadier symptom relief over several months, particularly where mechanical irritation and joint dryness are contributing to discomfort.
Key Benefits
- Supports joint lubrication and shock absorption
- Can reduce stiffness and improve joint movement
- May provide symptom relief for several months to a year
- Lower risk of cartilage impact compared to repeated steroids
- Suitable for patients wanting a non-steroid option
- Performed quickly in clinic, under ultrasound guidance
Potential Limitations
- Pain relief is not immediate and may take a few weeks
- Duration of benefit can vary between individuals
- May be less effective in more advanced osteoarthritis
- Typically requires a course of injections depending on the product used
- Can be more expensive than corticosteroid injections
Overall, hyaluronic acid injections can play a useful role within a broader rehabilitation-led management plan for knee osteoarthritis.
Arthrosamid® Injections
Unlike steroid or hyaluronic acid injections, it integrates into the synovial lining of the joint, forming a soft scaffold within the capsule.
This helps reduce the synovial irritation and inflammatory flare cycle that drives ongoing pain in knee OA.
Rather than wearing off over months, Arthrosamid® is designed to remain within the joint, with clinical data showing symptom relief that can last 2–5 years in appropriately selected patients.
Key Benefits
- Targets the synovial lining, helping reduce inflammatory flare-ups
- Long duration of effect (often 2–5 years)
- Single injection treatment
- Non-biodegradable hydrogel which remains within the joint
- Can delay the need for surgical intervention in some patients
- Can significantly improve pain, function and activity tolerance
Potential Limitations
- Higher upfront cost compared to steroid or hyaluronic acid injections
- Not suitable for every stage or presentation of knee OA
- Pain relief is not always immediate and may take several weeks
- It is more expensive treatment option
- Should still be combined with structured rehabilitation for best outcomes
- It does not regenerate cartilage
- It does not reverse osteoarthritis
When carefully selected and integrated into a wider physiotherapy-led plan, Arthrosamid® can provide a longer-term option within the conservative-to-surgical treatment pathway for knee osteoarthritis.
Who Is Arthrosamid® Suitable For?
Arthrosamid® is not necessarily the first-line treatment for knee OA.
At Complete Physio, we always prioritise:
- Structured physiotherapy
- Strengthening programmes
- Weight optimisation
- Activity modification
- Biomechanical assessmen
However, Arthrosamid® may be particularly helpful for patients who:
- Have symptomatic knee osteoarthritis
- Continue to experience flare-ups despite physiotherapy
- Have tried steroid injections, or Hyaluronic acid injections with limited success
- Are not ready for, or wish to delay, knee replacement surgery
- Do not yet have severe end-stage “bone-on-bone” arthritis
As with all treatments, earlier intervention in moderate OA often produces better outcomes than waiting until the joint is severely degenerated.
The Procedure: What to Expect
We ask all patients to provide written consent prior to booking an injection to ensure they have read and understood the information provided.
We do not require your doctor to refer you for an injection – However, we will supply you with a report after the procedure for you to forward to your GP or consultant for your medical records.
At Complete Physio, injections are performed by experienced clinicians, using ultrasound guidance for precision of needle placement and real time view of the knee joint.
The process typically involves:
- A clinical assessment and imaging review
- Cleaning and sterile preparation
- Local anaesthetic is used to ensure minimal discomfort
- The injection of Arthrosamid® is administered into the joint
- You will need to stay for a short observation period
The procedure usually takes around 20 – 30 minutes.
Aftercare and Recovery
Aftercare advice typically includes:
- Avoiding high-impact activity for several days after the injection
- Gentle mobility and normal movement of the knee is encouraged
- Applying ice and elevate the leg if mild swelling occurs
- Only resume a strengthening programme as guided by your physiotherapist
Some patients may experience:
- Temporary swelling of the knee
- Mild stiffness in the knee joint
- A short inflammatory response in the first few days which can sometimes increase pain
Improvement is not always immediate. Pain reduction is likely to develop gradually over a couple of weeks as the hydrogel integrates into the synovial lining.
The Main Benefits of Arthrosamid®
- It has a long-lasting effect (often 2–5 years in suitable cases)
- Reduces frequency and severity of inflammatory flare-ups
- Being non-biodegradable means it remains in situ within the joint
- Has the potential to delay or even eliminate the need for surgical intervention
It is more expensive than other injection options, but when viewed over a multi-year period, it compares favourably with repeated shorter-acting treatments, or the high cost of having surgery.
Where Does Arthrosamid® Fit in the Treatment Pathway?
At Complete Physio, we take a comprehensive and staged approach to knee osteoarthritis.
Step 1: Conservative Management
- Physiotherapy
- Strength training
- Movement retraining
- Education and load management
Step 2: Adjunctive Treatments
- Steroid injections
- Hyaluronic acid
- Arthrosamid®
Step 3: Surgical Referral
- When conservative and injection treatments are no longer sufficient – We work with some of the best consultants in London so will make sure you are provided with the best possible care.
Arthrosamid® sits between conservative care and surgery; it’s a useful “midpoint” option for the right patient.
Why Combine Arthrosamid® With Physiotherapy?
An injection alone rarely delivers the best long-term outcomes.
It is really important that patients also develop strong quadriceps, hamstrings and hip muscles to reduce the load going through the knee.
Improved flexibility and neuromuscular control also helps to decrease stress on the joint surfaces of your knee.
At Complete Physio, we integrate:
- Individualised rehab programmes
- Strength progression
- Biomechanical correction
- Ongoing monitoring
This combined approach gives our patients the best possible chance of sustained, measurable improvement, that maintains the active lifestyle they want.
Prognosis and Expectations
No treatment in medicine offers guarantees. Arthrosamid® does not work for everyone.
However, in appropriately selected patients with moderate osteoarthritis and recurrent inflammatory flares, results have shown that it can:
- Reduce knee pain
- Improve your mobility and function
- Decrease the severity and frequency of flare ups
- Delay or even eliminate the need for knee replacement surgery
The key is correct patient selection, ensuring realistic expectations are set, and that injection therapy is integrated with a rehabilitation programme.
Final Thoughts
Knee osteoarthritis is a progressive condition. However this progression does not mean inevitable surgery.
With the right blend of physiotherapy, load management and targeted injections such as Arthrosamid®, many patients can significantly improve symptoms and maintain activity levels for years.
If you are experiencing persistent knee pain or recurrent flare-ups despite undertaking a good rehabilitation programme, our clinical team at Complete Physio can assess whether Arthrosamid® may be appropriate for you as part of your treatment plan.
For more information you can visit the Arthrosamid® website here or download their brochure here.
Frequently Asked Questions (FAQs)
1. How quickly does Arthrosamid start working?
Improvement is often gradual. Some patients notice benefit within a few weeks, but optimal results typically develop over 6 – 12 weeks as the hydrogel integrates into the synovial lining.
2. How long does Arthrosamid last?
Clinical studies suggest benefits commonly last 2 – 5 years in appropriately selected patients.
3. Is Arthrosamid the same as a steroid injection?
No. Steroids reduce inflammation temporarily. Arthrosamid integrates into the synovial lining and works as a longer-term barrier against inflammatory flare-ups.
4. Will it regrow cartilage?
No. Arthrosamid does not regenerate cartilage or reverse osteoarthritis. It aims to reduce inflammation-driven symptoms and slow further inflammatory degradation.
5. Is the injection painful?
Most patients tolerate the procedure well. Local anaesthetic is used, and discomfort is typically mild and short-lived.
6. Are there side effects?
Temporary swelling, stiffness or mild inflammatory response may occur. Serious complications are uncommon when performed by experienced clinicians.
7. Can I still exercise after the injection?
Yes. Light activity is encouraged, but high-impact exercise should be avoided for several days. A structured strengthening programme is strongly recommended.
8. Who should not have Arthrosamid?
It may not be appropriate for patients with severe end-stage “bone-on-bone” arthritis, active joint infection, or significant structural instability.
References
- Bliddal, H., Hartkopp, A., Beier, J., Conaghan, P.G. and Henriksen, M., 2026. A prospective, open-label, clinical investigation of a single intra-articular polyacrylamide hydrogel injection in participants with knee osteoarthritis: A 5-year extension study. Journal of orthopaedic surgery and research, 21(1), p.43.
- Gao, H.C.K., Akhtar, M., Creedon, C., Nar, Ö.O., Verma, T. and Lee, P.Y., 2025. Polyacrylamide hydrogel injections in knee osteoarthritis: A PROMs-based 24 month cohort study. Journal of Clinical Orthopaedics & Trauma, 69.
- Bliddal, H., Beier, J., Hartkopp, A., Conaghan, P.G. and Henriksen, M., 2024. Effectiveness and safety of polyacrylamide hydrogel injection for knee osteoarthritis: results from a 12-month follow up of an open-label study. Journal of orthopaedic surgery and research, 19(1), p.274.
- Bliddal, H., Beier, J., Hartkopp, A., Conaghan, P.G. and Henriksen, M., 2024. Polyacrylamide gel versus hyaluronic acid for the treatment of knee osteoarthritis: a randomised controlled study. Clin Exp Rheumatol, 42(9), pp.1729-1735
- Bliddal, H., Beier, J., Hartkopp, A. and Conaghan, P., 2024. 3 YEAR FOLLOW-UP FROM A RANDOMISED CONTROLLED TRIAL OF INTRA-ARTICULAR POLYACRYLAMIDE HYDROGEL INJECTION IN SUBJECTS WITH KNEE OSTEOARTHRITIS. Osteoarthritis and Cartilage, 32(6), pp.770-771.
Don’t let pain hold you back, book now!





