What is an Achilles tendon rupture?
The Achilles tendon is a strong fibrous band that connects the calf muscles to the heel bone (calcaneus).
An Achilles rupture is when your tendon literally ‘snaps’ in two. It is also known as a complete tear of the Achilles. If you feel a ‘snap’ or ‘pop’ in the back of your heel, you may well have completely torn or ruptured your Achilles. This injury requires immediate medical attention. On occasion, the Achilles may have only partially torn. This is when some of the tendon fibres are still intact. A partial tear is very rare.
KEY POINT: if you have heard a ‘pop’ or felt a ‘snap’, it should always be treated as a rupture (a complete tear) until proven otherwise by an ultrasound or MRI scan.
An Achilles rupture is a common injury, particularly among athletes involved in sports that require explosive movements or sudden changes in direction, such as football and basketball. Performing these activities puts the Achilles tendon under high tension, which makes it susceptible to injury.
Surgery can be performed to repair the rupture but, for many people, non-surgical treatment can be equally as effective.
This article will help you better understand the causes, risk factors, symptoms, diagnosis, and treatment options for an Achilles tendon rupture.
Anatomy of the Achilles tendon
The Achilles tendon is the thickest, strongest and most powerful tendon in the human body.
It is the tendinous extension of the calf muscle (consisting of the soleus and the gastrocnemius muscles), inserting on the calcaneus.
What are the symptoms of an Achilles tendon rupture?
If your Achilles tendon ruptures, you might hear a ‘pop’ or feel a ‘snap’, followed by an immediate sharp pain in the back of your ankle and lower leg that is likely to affect your ability to walk properly. Some people liken the sensation to being ‘shot’ or ‘kicked’ in the calf.
If you are not sure if you have ruptured your Achilles you must see an experienced clinician as soon as possible. Any delay may adversely affect your long-term outcome.
The most common symptoms of an Achilles tendon rupture include:
- Sudden pain – a sharp and severe pain at the back of the ankle or calf.
- Swelling – rapid swelling in the area of the rupture, usually near the heel.
- Inability to stand on toes – difficulty or inability to rise onto the toes, or push off when walking on the affected side.
- Tenderness and bruising – there may be bruising around the ankle and foot and the tendon will be tender to touch.
- A palpable gap – when you touch your Achilles tendon you feel a gap, which may be hard to appreciate if you are not a trained clinician.
At Complete Physio we are experts in diagnosing and treating all Achilles tendon problems, from tendinopathy to ruptures. If you have experienced an injury and symptoms as described above, then it is vital that you do not delay getting a diagnosis and a treatment plan. Call us directly on 020 7482 3875 or email info@complete-physio.co.uk. We will ensure that you are seen as an urgent appointment, as soon as possible.
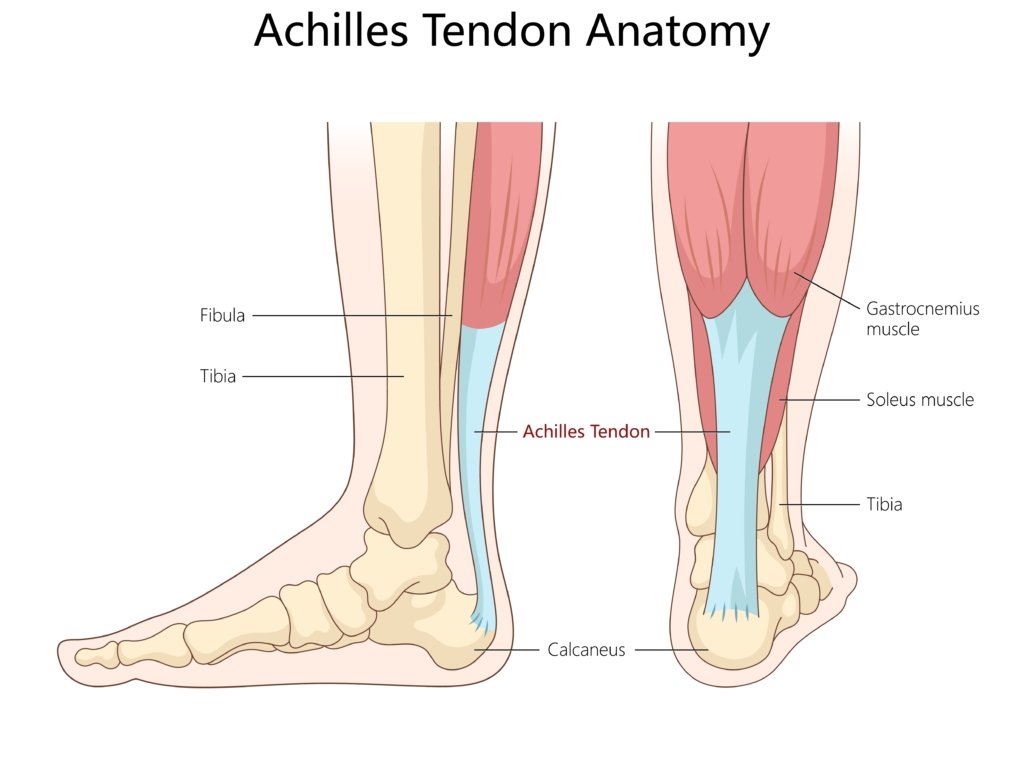
The main function of the Achilles tendon is the transmission of power from the calf muscles to the heel and the foot, enabling the foot to point forcefully downward (plantarflexion) and facilitate activities such as walking, running, and jumping.
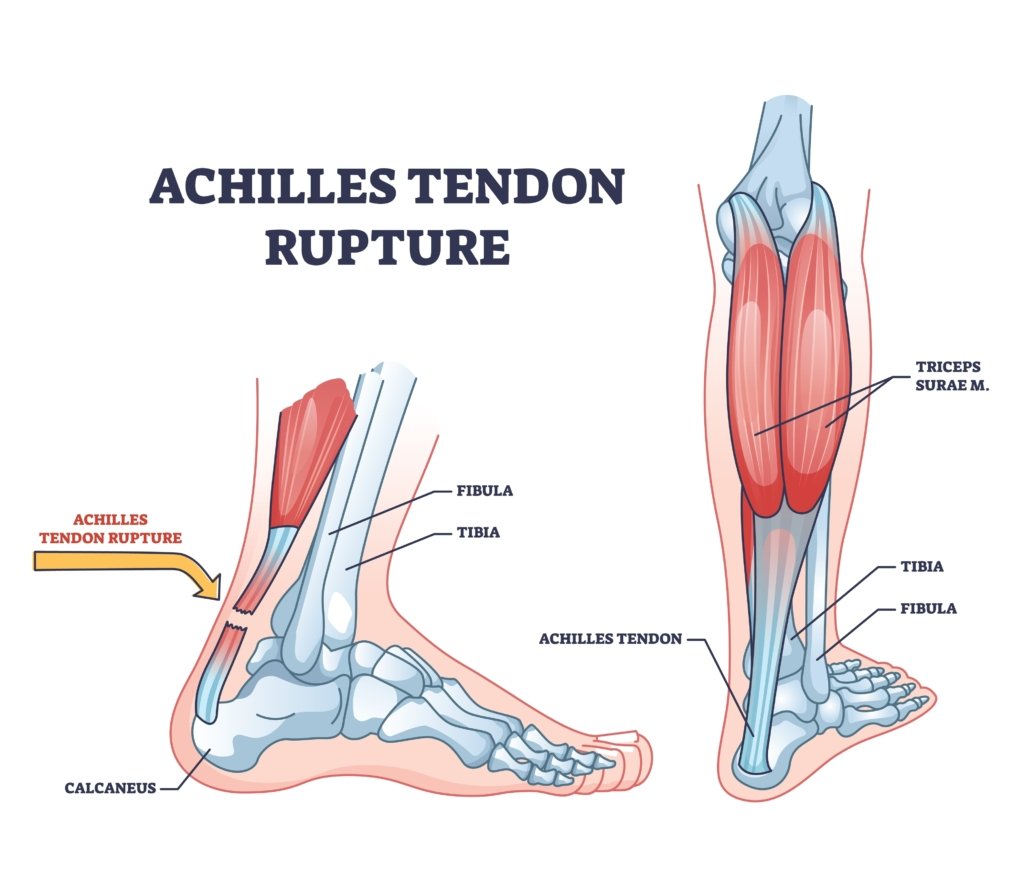
What causes an Achilles tendon rupture?
Achilles tendon ruptures often occur during activities that involve forceful pushing off from the foot while the knee is straight, such as during sprinting or jumping.
The Achilles tendon must withstand very high forces. For example, when running, a force up to eight times your bodyweight acts on the Achilles tendon. If there is any weakness in the tendon it can cause a tear or rupture.
Achilles tendon ruptures most commonly occur in the 30-50 year old male athlete, the weekend warrior playing a recreational game of football or tennis, or someone engaging in high level activity after a period of inactivity and deconditioning.
The most common causes include:
Sudden acceleration – a rapid increase in speed or change of direction, leading to excessive force on the tendon.
Trip or fall – a sudden trip or stumble, and your foot is thrust in front to break a fall, forcefully overstretching the tendon.
Direct trauma – a direct blow to the back of the ankle may contribute to an Achilles rupture.
Risk Factors
Certain factors may increase the risk of Achilles tendon ruptures, including:
- Age – ruptures are more common in individuals over the age of 30, as the tendon becomes less flexible and more prone to injury with age.
- Previous tendon injuries – individuals with a history of Achilles tendon problems such as Achilles tendinopathy are at higher risk.
- Gender: Achilles tendon ruptures are more common in men, likely due to higher participation in explosive sports, greater tendon stiffness, and the absence of the protective hormonal effects seen in pre-menopausal women.
- Certain medications – certain medications, such as taking steroids and some antibiotics, may increase the risk of tendon injury.
- Increased activity – doing more exercise than you are used to, or increasing the amount you do too quickly.
- Obesity – excess weight puts more strain on the tendon.
- Systemic inflammation caused by obesity – Obesity is associated with chronic low-grade systemic inflammation and increased mechanical load on the Achilles tendon, both of which can impair tendon health and increase the risk of rupture.
- Increased cholesterol – Elevated cholesterol levels can lead to fatty deposits within tendons, reducing tendon strength and elasticity and making the Achilles tendon more vulnerable to injury and rupture.
- Diabetes – type 1 diabetes, in particular, predisposes to an increased rupture rate.
- Ethnicity – certain ethnicities have an increased rate of Achilles ruptures.
What are the symptoms of an Achilles tendon rupture?
If your Achilles tendon ruptures, you might hear a ‘pop’ or feel a ‘snap’, followed by an immediate sharp pain in the back of your ankle and lower leg that is likely to affect your ability to walk properly. Some people liken the sensation to being ‘shot’ or ‘kicked’ in the calf.
If you are not sure if you have ruptured your Achilles you must see an experienced clinician as soon as possible. Any delay may adversely affect your long-term outcome.
The most common symptoms of an Achilles tendon rupture include:
- Sudden pain – a sharp and severe pain at the back of the ankle or calf.
- Swelling – rapid swelling in the area of the rupture, usually near the heel.
- Inability to stand on toes – difficulty or inability to rise onto the toes, or push off when walking on the affected side.
- Tenderness and bruising – there may be bruising around the ankle and foot and the tendon will be tender to touch.
- A palpable gap – when you touch your Achilles tendon you feel a gap, which may be hard to appreciate if you are not a trained clinician.
How do we diagnose an Achilles tendon rupture?
Watch this video for more information about how we diagnose an Achilles tendon rupture.
Clinical Assessment
It is essential to get an early and accurate diagnosis of your problem to ensure that you are started on the best and most effective treatment plan. A diagnosis will be made by one of our expert physiotherapists.
The rate of misdiagnosis is high, but fortunately at Complete Physio our physiotherapists are highly experienced, methodical and thorough in their assessment.
They will ask questions about your injury, symptoms, past health, and exercise regime to assist making a diagnosis.
After the history is taken, your specialist will complete a series of physical tests to confirm their diagnosis.
Depending on your pain levels this may include:
- Gently, but skilfully, feeling your Achilles tendon from top to bottom. There is often (but not always) a palpable gap in the Achilles tendon when it is ruptured.
- Thompson Test – a simple test where the calf is squeezed to check for foot movement, which is absent in cases of a complete rupture. This test has a sensitivity of 96% and specificity of 93%.
- Measuring the range of movement of your ankle.
- Assessing the muscle strength of your calf.
- Watching you walk and assessing your ability to push off on your toes.
Imaging Tests
Imaging tests, such as MRI or diagnostic ultrasound, are commonly used to confirm the diagnosis and assess the extent of the injury.
Diagnostic ultrasound is the gold standard imaging tool for assessing tendon structure in the Achilles. It is superior to MRI for this condition and many other tendon complaints.
An ultrasound scan is the imaging modality of choice as it provides immediate information and can be carried out in the clinic room. It is also more cost effective than an MRI for self-funding patients.
Furthermore, it can be used dynamically (unlike an MRI scan) i.e. you can image the tendon whilst moving the ankle to observe if the end of the tendons can be brought back together or if a significant gap remains. This can be very important when determining if surgery is required.
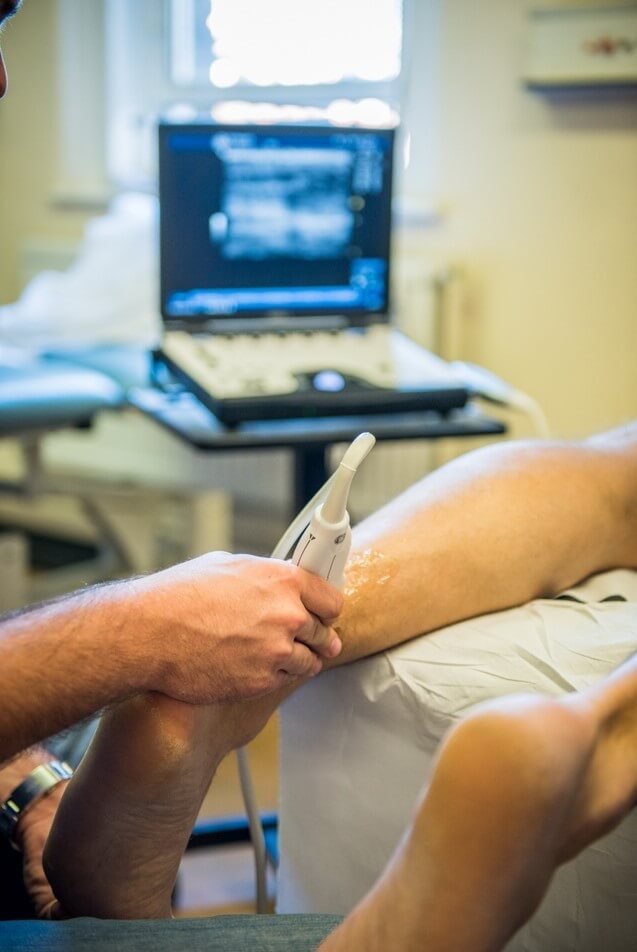
At Complete Physio we are able to offer a unique, one-stop service that sets us apart from other physiotherapy and sports injury clinics.
We have a team of dual qualified physiotherapists and sonographers who can carry out an ultrasound scan as part of your clinical assessment and will provide a comprehensive report.
Gaining more information about exactly which part of the tendon is affected and the severity of the tear is important in order to implement the most effective treatment plan for your specific needs.
You do not require a GP referral, and we do not charge extra for an ultrasound scan. However, you will need to be booked in with one of our Clinical Specialists, so please ensure you inform our administration team that you would like to have an ultrasound scan at the time of booking.
How do we treat a ruptured Achilles?
Treatment options for an Achilles tendon rupture include both surgical and non-surgical approaches.
If you are unlucky enough to be diagnosed with an Achilles tendon rupture you will need to seek immediate treatment from an appropriately trained clinician. At Complete Physio we work very closely with some of the top foot and ankle orthopaedic consultants in the country and can refer you directly if required.
To find out more about whether you should have your Achilles surgically repaired or not, you can watch our very popular Complete Physio Podcast, with our Clinical Director and Achilles expert, Chris Myers and consultant orthopaedic surgeon, Mr Sam Singh. Between them they see hundreds of Achilles injuries every year! This is a must watch if you have ruptured your Achilles.
Non-surgical treatment (also known as “conservative treatment”)
This will involve immobilisation of the ankle in a below knee plaster cast (also known as a ‘backslab’) or walking boot. You will be walking with the aid of elbow crutches for several months to allow the tendon to heal naturally.
Initially in A&E, you may be given a plaster cast for 1-2 weeks. On occasion, you may be given a walking boot straight away. It just depends on the protocol of the clinic or hospital. Whether it is a plaster cast or walking boot, you will struggle to put weight on your leg and you will need to use crutches or a ‘knee walker’ to move around.
The cast or boot is used to ensure your foot is in a ‘pointed down position’ (what is called a ‘plantarflexed’ position) as quickly as possible after your injury. Getting your foot into a ‘pointed down’ position as soon as possible is a key component to ensure optimal healing, and will help avoid the development of long-term issues.
It is also essential to keep the cast or walking boot on at all times, even at night. Yes, 24 hours a day! You normally have the boot on for 8-12 weeks depending on the protocol of your clinic, consultant or hospital. Protocols do vary.
The walking boot is a rigid type of boot made from plastic with velcro straps to adjust it. The angle of your foot can be adjusted within the walking boot over a number of weeks, so you move from the foot ‘pointed down’ position to a more neutral position over time. The change of angle is essential to ensure the tendon heals correctly. As the weeks pass you will be able to put weight on your injured side and start your rehabilitation. This must be guided by your physiotherapist.
There are two types of walking boots; the Aircast Boot and the VACOped. They are both rather awkward to wear initially, but you do get used to them. Both walking boots provide the necessary support and angle adjustment, but we prefer the VACOped as it maintains the ankle in a more optimal plantarflexed position.
We would always recommend you use an “EVEN up” to level up your leg length when walking with a boot on. This will prevent unwanted pains in your lower back hip and leg. They can be purchased online here.
Aircast boot
VACOped Boot
For more information we have a selection of useful videos on YouTube on our Achilles ‘playlist’ including how to walk with a boot on, how to use elbow crutches, and how to go upstairs and downstairs with crutches.
We also have a very useful video demonstrating what exercises you CAN do with the boot on!
Non-surgical treatment will be discussed with you at the time of the injury. Together with your orthopaedic surgeon and/or physiotherapist, you will decide which option is best for you. In the UK, non-surgical treatment is the most common route and is sometimes the only option presented to you in A&E. Surgical treatment is reserved for younger, more active individuals who endeavour to return to sports such as sprinting, football, rugby, and basketball.
Compared to surgery, non-surgical treatment has a lower chance of complications, as you avoid the potential (but unlikely) risks of surgery, such as infection. However, in some studies it has been reported there is a greater chance of having another rupture in the future, known as a re-rupture, if you opt for non-surgical treatment. This has not been replicated in all clinical trials. From experience, if you opt for non-surgical treatment and diagnosis and treatment is delayed or sub-optimal, you have an increased risk of poor tendon healing and ‘lengthening’ of the tendon which can result in poor calf function and an inability to return to sport at your pre-injury levels.
Listen to our Podcast for more information about ‘lengthening’.
Surgical Treatment for Achilles rupture
Surgery may be recommended, especially for more active individuals and athletes, to repair the torn tendon and restore strength and function.
Your doctor may be more likely to suggest surgery if:
- You are young and active
- You are a competitive athlete
- You had a delay in diagnosis and treatment of the rupture
- You have previously ruptured your Achilles tendon
- An ultrasound scan or MRI reveals significant retraction of one end of the tendon or a large gap (generally greater than 1 cm) between the two ends of the tendon.
There are several different techniques for surgical repair of the Achilles tendon; all involve bringing the torn ends of your tendon back together.
Most surgeons will use a minimally invasive (key hole) approach, but sometimes if the surgery is more complex, you may have open surgery, which involves making a slightly larger incision to fix the tendon.
Your surgeon will explain the different surgical options, so you can decide what’s best for you.
After your operation, you may be placed into a cast, but will quickly be progressed into a walking boot to help the tendon heal.
A similar protocol to non-surgical management is often followed after your surgery i.e. you will wear a walking boot for 8-12 weeks and use elbow crutches, but this will depend on your surgeon’s protocol.
Physiotherapy and Rehabilitation
Whether you had surgery for your Achilles tendon or not, physiotherapy plays a crucial role in the recovery and rehabilitation process following an Achilles tendon rupture.
Your surgeon will refer you to Complete Physio, usually 2-3 weeks following your injury or operation.
Your physiotherapist will guide you through the post-operative protocol and the correct exercises to strengthen your calf, ankle and lower leg.
You will start with some basic strengthening exercises, designed to restore normal calf muscle bulk and strength, which will be progressed over time.
It is very important you DO NOT STRETCH your calf and Achilles, otherwise you will end up with a ‘long’ tendon and a sub-optimal outcome.
Your physiotherapist may also advise you on what low-impact exercises, such as cycling, jogging or swimming, you can try.
At Complete Physio all our clinicians have extensive experience of Achilles ruptures, both surgical and non-surgical management.
Physiotherapy treatment will include:
Walking training (known as gait re-education)
Your physiotherapist will teach you how to walk again and will give you exercises to improve your technique (so you don’t limp too much) and walking tolerance. They will take away the ‘fear’ elements that may develop following this injury.
Reducing swelling and pain
Techniques like ice, compression, and elevation can be used to reduce inflammation and alleviate pain.
Restoration of range of motion
Gentle stretching exercises are introduced to improve the flexibility of the hip, knee and ankle.
HOWEVER, YOU WILL NOT BE ASKED TO STRETCH YOUR ACHILLES TENDON.
Your physiotherapist may also apply some ‘hands on’ techniques to help reduce your swelling and improve circulation.
Strengthening exercises
Gradual strengthening exercises are prescribed to rebuild the strength of the calf muscles and the healing tendon. This is a key component of your treatment programme.
Manual Therapy
Your physiotherapist may use manual therapy such as massage or soft tissue release techniques to the surrounding muscles and incision site. This will help improve movement and reduce muscle stiffness or soreness.
Functional Exercises
Specific exercises are incorporated to improve balance, proprioception, and gait patterns to restore normal movement. Functional training can help you safely resume more demanding activities and get you back to playing the sport that you love and minimise your chance of future injury.
Recovery from Achilles tendon rupture
The success of treatment following an Achilles tendon rupture will depend on many factors.
They include:
- The quality of the surgical repair (if you have had surgery)
- Your adherence to using the walking boot and the whole treatment protocol
- The quality and experience of your physiotherapist
- Your commitment to rehabilitation and adherence to the prescribed exercises
- Your overall health and fitness at the time of the injury.
With expert physiotherapy, most patients can regain full strength, flexibility, and return to their normal activities/sports.
How long it takes to recover from an Achilles tendon rupture is similar whether you opt for surgical or non-surgical management.
You can expect to be back to normal activities and low-impact activity within four to six months, but it can take longer to get back to high-impact, explosive sports, such as football, squash or tennis – approximately 6-12 months.
In most cases you will be able to return to the type of activity and level that you did before your injury. But if you play sport at a professional level, you may find some limitations in what you can do. You will need a highly specialised team to get back to your previous level of performance, and it may take closer to 1 year.
At Complete Physio we are experts in treating Achilles tendon problems, including tendon ruptures. We use the latest evidence-based techniques and personalised treatment plans to ensure that you reach your goals.
We are dedicated to getting you back to full function and back to doing all the activities and sports that you enjoy.
For more information we have a selection of useful videos on our Achilles ‘playlist’ on YouTube.
Here are some common questions we get asked about Achilles tendon ruptures:
Q1: Can an Achilles tendon rupture heal on its own without surgery?
Yes. In the majority of cases, non-surgical treatment with immobilisation (in a walking boot) and physiotherapy lead to satisfactory healing and return to full function.
Q2: How long does it take to recover from an Achilles tendon rupture with surgical and non-surgical management?
The recovery period after a rupture varies greatly but typically ranges from six months to a year, depending on the extent of the injury and the patient’s dedication to rehabilitation. This is similar whether you have surgery or non-surgical management.
Q3: Can I return to sports after an Achilles tendon rupture?
Yes. Many individuals return to sports and physical activities after a full recovery and completion of a comprehensive physiotherapy programme, whether you have surgery or non-surgical management.
Q4: Is physiotherapy necessary after surgery for an Achilles tendon rupture?
Yes, physiotherapy is essential after surgery to promote healing, regain strength, and restore normal function of the ankle and calf.
Q5: Can Achilles tendon ruptures be prevented?
While some factors, such as age and gender, cannot be controlled, maintaining strong calf muscles, proper warm-up before physical activities, plus maintaining a healthy weight, diet and lifestyle to manage the load going through the tendon MAY help reduce the risk of Achilles tendon ruptures.
Click here for more questions and answers about Achilles tendon ruptures.
References:
- Egger, A.C. and Berkowitz, M.J., 2017. Achilles tendon injuries. Current reviews in musculoskeletal medicine, 10(1), pp.72-80.
- Owens, B., Mountcastle, S. and White, D., 2007. Racial differences in tendon rupture incidence. International journal of sports medicine, 28(07), pp.617-620.
- Amin, N.H., Old, A.B., Tabb, L.P., Garg, R., Toossi, N. and Cerynik, D.L., 2013. Performance outcomes after repair of complete Achilles tendon ruptures in National Basketball Association players. The American journal of sports medicine, 41(8), pp.1864-186
- Renninger, C.H., Kuhn, K., Fellars, T., Youngblood, S. and Bellamy, J., 2016. Operative and nonoperative management of Achilles tendon ruptures in active duty military population. Foot & ankle international, 37(3), pp.269-273.
- Horstmann, T., Lukas, C., Merk, J., Brauner, T. and Mündermann, A., 2012. Deficits 10-years after Achilles tendon repair. International journal of sports medicine, 33(06), pp.474-479.
- Zellers, J.A., Carmont, M.R. and Silbernagel, K.G., 2016. Return to play post-Achilles tendon rupture: a systematic review and meta-analysis of rate and measures of return to play. British journal of sports medicine, 50(21), pp.1325-1332.
- Porter, M.D. and Shadbolt, B., 2015. Randomized controlled trial of accelerated rehabilitation versus standard protocol following surgical repair of ruptured Achilles tendon. ANZ journal of surgery, 85(5), pp.373-377.
- Clanton, T.O., Haytmanek, C.T., Williams, B.T., Civitarese, D.M., Turnbull, T.L., Massey, M.B., Wijdicks, C.A. and LaPrade, R.F., 2015. A biomechanical comparison of an open repair and 3 minimally invasive percutaneous Achilles tendon repair techniques du
- McMahon, S.E., Smith, T.O. and Hing, C.B., 2011. A meta-analysis of randomised controlled trials comparing conventional to minimally invasive approaches for repair of an Achilles tendon rupture. Foot and ankle surgery, 17(4), pp.211-217.
Don’t let pain hold you back, book now!