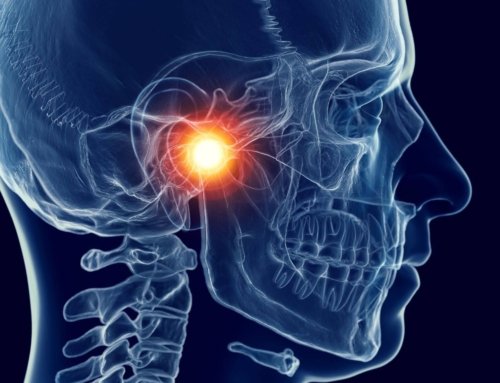
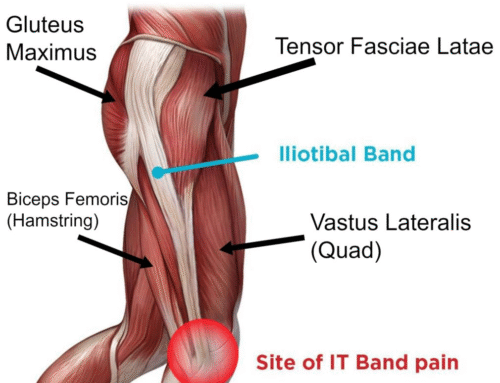
Clinical review: Lachlan Sutton, Clinical Specialist in Chronic Pain, Complete Physio.
Chronic pain is pain that persists beyond 12 weeks and is usually no longer caused by tissue damage. In most cases, the nervous system itself becomes sensitised, producing real pain signals without ongoing injury.
Physiotherapy-led treatment combining graded exercise, education, and lifestyle modification helps 70-80% of patients reduce symptoms significantly within 3-6 months.
Around 28 million adults in the UK live with chronic pain.
If you’ve been dealing with pain for months, or even years, and tests keep coming back “normal,” you’re not imagining it.
Persistent pain is one of the most misunderstood conditions in healthcare, and getting the right explanation is often the first step toward improvement.
Here’s what the latest evidence shows about why pain persists and what actually helps.
Key Takeaways
- Tissue damage isn’t the culprit. Chronic pain isn’t about tissue damage. After 12 weeks, most injuries have healed. Persistent pain is usually driven by nervous system sensitisation. The nervous system’s alarm becomes overactive.
- Central sensitisation represents genuine neurological changes. Central sensitisation means your body’s alarm system is turned up too high, increasing sensitivity to non-harmful stimuli. This reflects measurable brain activity rather than psychological factors alone.
- Exercise remains the most effective treatment. Consistency and gradual progression outperform sporadic intense sessions.
- Sleep and stress significantly impact pain thresholds. Both poor sleep and high stress affect neural pathways involved in pain perception and require simultaneous management.
- Recovery is achievable. The body is bioplastic and the nervous system can be rewired. A specialist chronic pain physiotherapist can identify the specific drivers of your pain and build a targeted recovery plan. With the right combination of education, graded exercise, and lifestyle changes, most chronic pain patients see some improvement within 8-12 weeks.
What qualifies as chronic pain?
Chronic pain is any pain that persists beyond the normal tissue healing time – typically longer than 12 weeks.
In acute injuries, pain serves a protective purpose. If you break your leg, pain stops you from walking on it and causing further damage. This is helpful and necessary.
Most soft tissue injuries heal within 6-12 weeks.
When pain persists beyond this window, something different is happening. As Lachlan Sutton, Complete Physio’s chronic pain specialist, explains:
“The vast majority of persistent pain cases are usually to do with changes within people’s nervous system (central sensitisation) and changes within the musculoskeletal system – increased guarding, bracing, and putting more stress on other structures.”
- Acute pain (0-12 weeks): Usually linked to tissue injury, serves a protective function
- Chronic pain (12+ weeks): Pain persists after tissues have healed; driven by nervous system sensitisation
- Key difference: Chronic pain can be severe, but it rarely indicates ongoing structural damage
What Causes Chronic Pain? The Science Behind It
Chronic pain is primarily caused by central sensitisation – where your nervous system’s “volume control” gets turned up and stays up.
Think of your nervous system as an alarm system; in a healthy state, it fires when there’s a genuine threat. In chronic pain, the alarm becomes hypersensitive, triggering at lower and lower thresholds.
This isn’t psychological, it’s a measurable neurological change.
This can manifest in 3 different ways:
- Hyperalgesia – An increased pain response to painful stimuli.
- Allodynia – Pain resulting from stimuli that are usually non-painful (e.g., light touch).
- Expanded Receptive Fields – Pain experienced in an area, away from the initial injury site.
Several factors contribute to this sensitisation:
- Neural pathway changes: Repeated pain signals strengthen nerve pathways, making them fire more easily. This process is known as long-term potentiation (LTP).
- Reduced inhibition: Your brain’s natural pain-dampening systems become less effective
- Muscle guarding: Protective tension around the painful area creates secondary strain on surrounding structures
- Sleep disruption: Poor sleep reduces your body’s ability to regulate pain — creating a vicious cycle
- Stress and anxiety: Psychological distress amplifies pain signals through shared neural pathways. This includes fears related to the injury/pain itself.
What Is the Best Treatment for Chronic Pain?
The most effective chronic pain treatment combines graded exercise, education, and addressing lifestyle factors like sleep and stress, rather than rest or repeated tests and scans.
One of the most important shifts in chronic pain understanding is moving away from a purely structural model.
As our chronic pain specialist puts it:
“We’re not just looking at a sore knee or a sore back. We’re looking at the whole person; what’s their sleep like, what’s their stress like, what’s their general health like.”
Evidence-based approaches include:
- Graded exposure and exercise: Gradually increasing activity levels to show the nervous system that movement is safe
- Pain education: Understanding what’s driving your pain reduces fear and catastrophising – two major amplifiers of pain
- Sleep optimisation: Improving sleep quality has a direct measurable effect on pain thresholds
- Interventions such as CBT (cognitive behavioral therapy) or CFT (cognitive functional therapy) with a chronic pain specialist: Assessing biological, psychological and social factors contribute to pain. CBT looks to understand and alter any beliefs which may be affecting our behaviour (ie belief that pain means damage leading to fear and avoidance of movement).
CFT takes a similar biopsychosocial approach with a specific focus on assessing and retraining movement and postures associated with pain. Often looking to restore preinjury movement to reduced pain induced muscle guarding.
- Sleep optimisation: Improving sleep quality has a direct measurable effect on pain thresholds
- Interventions such as CBT (cognitive behavioral therapy) or CFT (cognitive functional therapy) with a chronic pain specialist: Assessing biological, psychological and social factors contribute to pain. CBT looks to understand and alter any beliefs which may be affecting our behaviour (i.e. belief that pain means damage leading to fear and avoidance of movement). CFT takes a similar biopsychosocial approach with a specific focus on assessing and retraining movement and postures associated with pain. Often looking to restore preinjury movement to reduced pain induced muscle guarding.
- Hands-on treatments: Such as manual therapy to reduce muscle guarding and improve movement confidence. Acupuncture or TENS
- Appropriate medications prescribed by knowledgeable clinicians can be an integral part of a larger treatment plan.
Does Living with Chronic Pain Change Your Brain?
Yes, chronic pain produces measurable changes in brain structure and function, but these changes are reversible with the right treatment.
Research using brain imaging has shown that persistent pain can alter the areas of the brain responsible for processing pain signals, emotions, and decision-making.
This is why chronic pain often comes with fatigue, difficulty concentrating, and mood changes, it’s not “just” pain.
The encouraging news – studies show that effective pain management, particularly exercise and education-based approaches, can reverse these brain changes.
The nervous system is plastic, meaning it can be retrained.
Key finding: Patients who complete a structured chronic pain physiotherapy programme show measurable improvements in brain function within 8-12 weeks – mirroring the timeframe of nervous system adaptation.
When Should You See a Chronic Pain Physiotherapist?
See a chronic pain specialist if your pain has persisted beyond 3 months, you’ve had investigations that show no clear structural cause, or your pain is spreading to new areas.
Lachlan identifies several key indicators that suggest you would benefit from specialist chronic pain physiotherapy:
- Pain lasting longer than 12 weeks despite standard treatment
- Scans and tests coming back “normal” despite significant pain
- Pain that seems disproportionate to any identified injury
- Pain spreading to areas beyond the original site
- Increasing sensitivity to touch, temperature, or pressure
- Sleep disruption, fatigue, or mood changes alongside pain
- Fear of movement or avoidance of activities you used to enjoy
“If we can manage acute injuries well and prevent persistent pain from developing in the first place, it’s a whole lot easier,” Lachlan adds. “But even when it’s established, there’s always something that can be done.”
How Does Physiotherapy for Chronic Pain Work?
Chronic pain physiotherapy works by systematically addressing the multiple factors driving your pain – not just treating a single body part.
Unlike standard physiotherapy that focuses on a specific joint or muscle, chronic pain treatment takes a biopsychosocial approach.
This means looking at biological factors (nervous system sensitisation, deconditioning), psychological factors (fear of movement, catastrophising, stress), and social factors (work demands, relationships, support networks).
A typical treatment programme at Complete Physio includes:
- Comprehensive assessment: Understanding your pain history, lifestyle, sleep, stress, and movement patterns
- Pain education: Helping you understand what’s driving your specific pain. Addressing unhelpful beliefs, movement fear-avoidance, catastrophizing, and emotional distress associated with pain. This alone reduces severity in many patients.
- Graded exercise programme: Starting where you are and progressively building capacity and confidence
- Lifestyle modification: Targeted changes to sleep, stress management, and daily activity pacing
- Hands-on treatments: Where appropriate, to de-sensitise tissues, address muscle tension, reduce pain, and improve movement quality.
- Self-management tools: Building your own toolkit so you can manage flare-ups independently
Can Exercise Make Chronic Pain Worse?
Exercise done correctly does not make chronic pain worse – but the wrong type, intensity, or approach can temporarily increase symptoms.
This is one of the biggest fears for chronic pain patients, and it’s understandable. When movement hurts, your instinct is to stop.
But as Lachlan explains: “Exercise is one of the single most important things for chronic pain. The key is getting the dosage right.”
The principles of exercise for chronic pain:
- Start low: Begin well within your current tolerance – even if that means just walking for 5 minutes
- Progress gradually: Increase by small increments (10-15% per week maximum)
- Expect some discomfort: Mild pain during or after exercise doesn’t mean damage – it means your alarm system is still sensitive
- Consistency over intensity: Regular moderate activity is far more effective than occasional intense sessions
- Variety matters: Combining cardiovascular exercise, strengthening, and flexibility work produces the best outcomes
Focus on ‘how’ you move: Avoid forcing movements which make the body ‘tense up’ and remembering to control your breathing throughout. The goal is to train the body to move in a relaxed way rather than learning to tighten muscles more.
Frequently Asked Questions
Is chronic pain all in my head?
No. Chronic pain is a real neurological condition involving measurable changes in how your nervous system processes signals. While psychological factors like stress and anxiety can amplify pain, the pain itself is not imagined. It is produced by a sensitised nervous system, and effective treatment addresses all contributing factors.
How long does it take for chronic pain physiotherapy to work?
Most patients see meaningful improvement within 8-12 weeks of consistent treatment. Some notice changes in pain understanding and movement confidence within the first few sessions. Full recovery timelines vary depending on how long the pain has been present and how many contributing factors are involved.
Do I need a scan or MRI for chronic pain?
In most chronic pain cases, scans are not helpful and can sometimes be counterproductive. Many scan findings (disc bulges, wear and tear) are normal age-related changes found in pain-free people too. A thorough clinical assessment by a specialist physiotherapist is usually more informative than imaging.
Can chronic pain go away completely?
Yes, many people fully recover from chronic pain. Because persistent pain is driven by nervous system sensitisation rather than tissue damage, the nervous system can be retrained through graded exercise, education, and lifestyle changes. The degree of recovery depends on individual factors, but significant improvement is achievable for the vast majority.
What is central sensitisation?
Central sensitisation is a condition where the central nervous system amplifies danger signals, making you more sensitive to stimuli that wouldn’t normally be painful. It is the primary mechanism behind most chronic pain conditions. Think of it as your pain alarm system being stuck on high, the alarm is real, but the threat level it’s responding to is exaggerated.
Should I stop exercising if it hurts?
Not necessarily. With chronic pain, some discomfort during and after exercise is expected because your nervous system is sensitised. Pain during exercise does not mean you’re causing damage. The key is working with a specialist to find the right starting level and progressing gradually. Stopping all activity typically makes chronic pain worse over time.
What is the difference between a chronic pain physio and a normal physio?
A chronic pain physiotherapist has additional training in pain neuroscience, central sensitisation, and the biopsychosocial model of pain. They assess the whole person; sleep, stress, psychology, lifestyle, not just the painful body part. Standard physiotherapy typically focuses on structural rehabilitation, which is less effective for established chronic pain.
Does stress make chronic pain worse?
Yes. Stress activates the same neural pathways as physical pain, directly increasing nervous system sensitisation. High stress levels reduce your pain threshold, meaning stimuli that might not bother you on a good day can become genuinely painful when you’re under pressure. Stress management is a core component of effective chronic pain treatment.
Conclusion
Chronic pain is not about damage, it’s about a sensitised nervous system that needs retraining. The combination of pain education, graded exercise, sleep improvement, and stress management is the most evidence-backed approach, and it works for the majority of patients.
If you’ve been living with persistent pain and haven’t found answers, a specialist chronic pain physiotherapist can help identify exactly what’s driving your symptoms and build a clear plan to address them.
Book a consultation with our chronic pain specialist or call us on 020 7482 3875.
References
- NICE Guidelines: Chronic Pain Assessment and Management (NG193)
- Moseley, G.L. and Butler, D.S., 2015. Fifteen Years of Explaining Pain: The Past, Present, and Future. The Journal of Pain, 16(9), pp.807-813
- Nijs, J., George, S.Z., Clauw, D.J., Fernandez-de-las-Penas, C., Kosek, E., Ickmans, K., Fernandez-Carnero, J., Polli, A., Kapreli, E., Huysmans, E. and Cuesta-Vargas, A., 2021. Central sensitisation in chronic pain conditions: latest discoveries and their potential for precision medicine. Lancet Rheumatology, 3(5), pp.E383-E392
- Geneen, L.J., Moore, R.A., Clarke, C., Martin, D., Colvin, L.A. and Smith, B.H., 2017. Physical activity and exercise for chronic pain in adults: an overview of Cochrane Reviews. Cochrane database of systematic reviews, (4).
- Borsook, D., Youssef, A.M., Simons, L., Elman, I. and Eccleston, C., 2018. When pain gets stuck: the evolution of pain chronification and treatment resistance. Pain, 159(12), p.2421.
- O’Sullivan PB, Caneiro JP, O’Keeffe M, Smith A, Dankaerts W, Fersum K, O’Sullivan K. Cognitive Functional Therapy: An Integrated Behavioral Approach for the Targeted Management of Disabling Low Back Pain. Phys Ther. 2018 May 1;98(5):408-423.
Don’t let pain hold you back, book now!