Temporomandibular Joint (TMJ) Dysfunction
If you’re experiencing jaw pain, clicking, or difficulty opening your mouth, it might well be that you have a problem with your Temporomandibular Joint (TMJ) - a surprisingly common issue that can have a huge impact on your daily life.
Whether you are getting pain when chewing, suffering from tension headaches, or finding that your jaw feels locked or clicks, TMJ problems can be incredibly frustrating, and sometimes quite debilitating.
At Complete, we understand how debilitating TMJ pain can be.
What is TMJ Dysfunction?
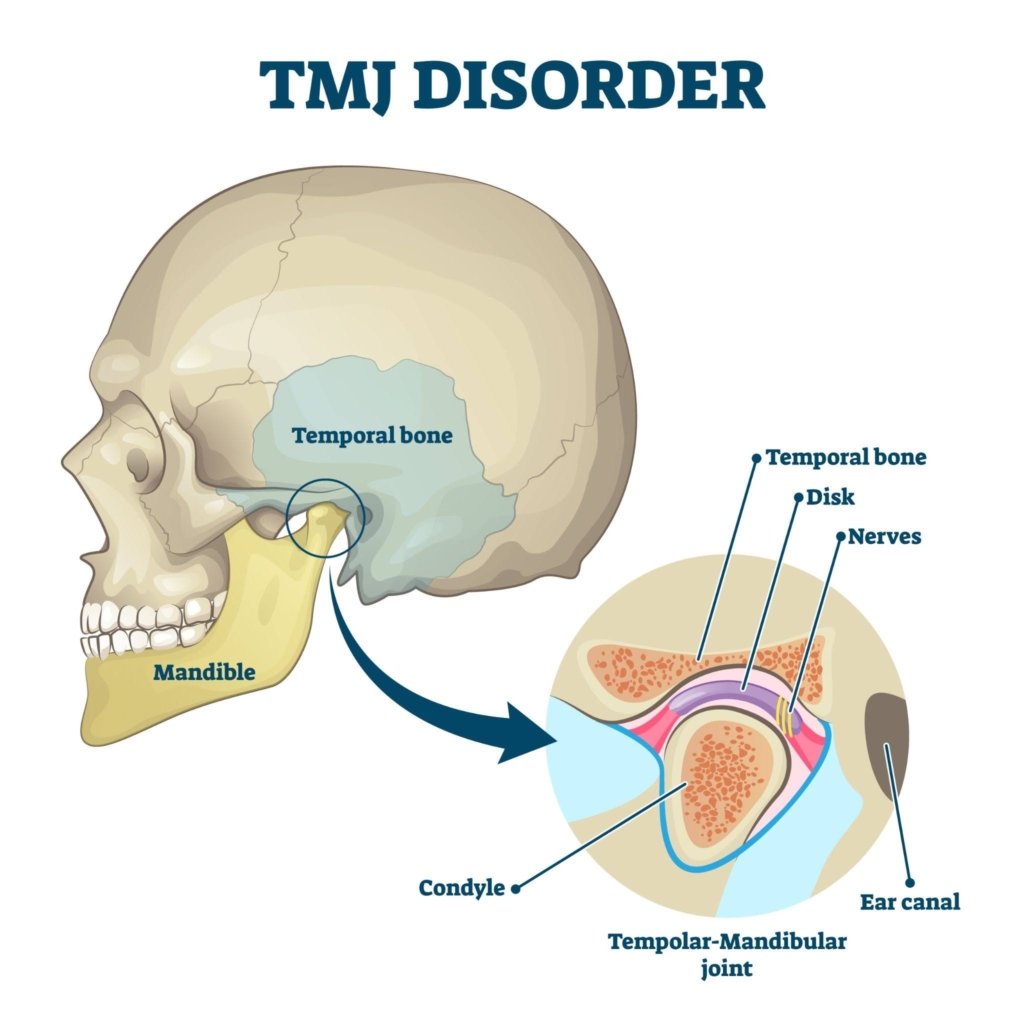
Your Temporomandibular Joint (TMJ) is the small but very powerful hinge that connects your jawbone (mandible) to your skull. It sits just in front of your ear on each side of your face and allows you to talk, chew, yawn, sing, and make facial expressions.
Unlike other joints in the body, the TMJ is unique - it doesn’t just hinge up and down but also slides forward, backward, and side to side. This complex movement makes it incredibly versatile but also vulnerable to problems.
When the TMJ isn’t functioning properly; whether due to inflammation, muscle tightness, joint damage, or postural issues, it can cause pain, clicking, restricted movement, and even headaches or ear discomfort.
Understanding the Anatomy of the TMJ
Bones & Cartilage
The TMJ is made up of the mandible (lower jaw) and the temporal bone (part of the skull). Between the bones is a disc of cartilage, which acts as a shock absorber and helps the joint to glide smoothly when you open and close your mouth to chew or speak. If this disc moves out of place or wears down, it can cause clicking, popping, or even locking.
Muscles & Ligaments
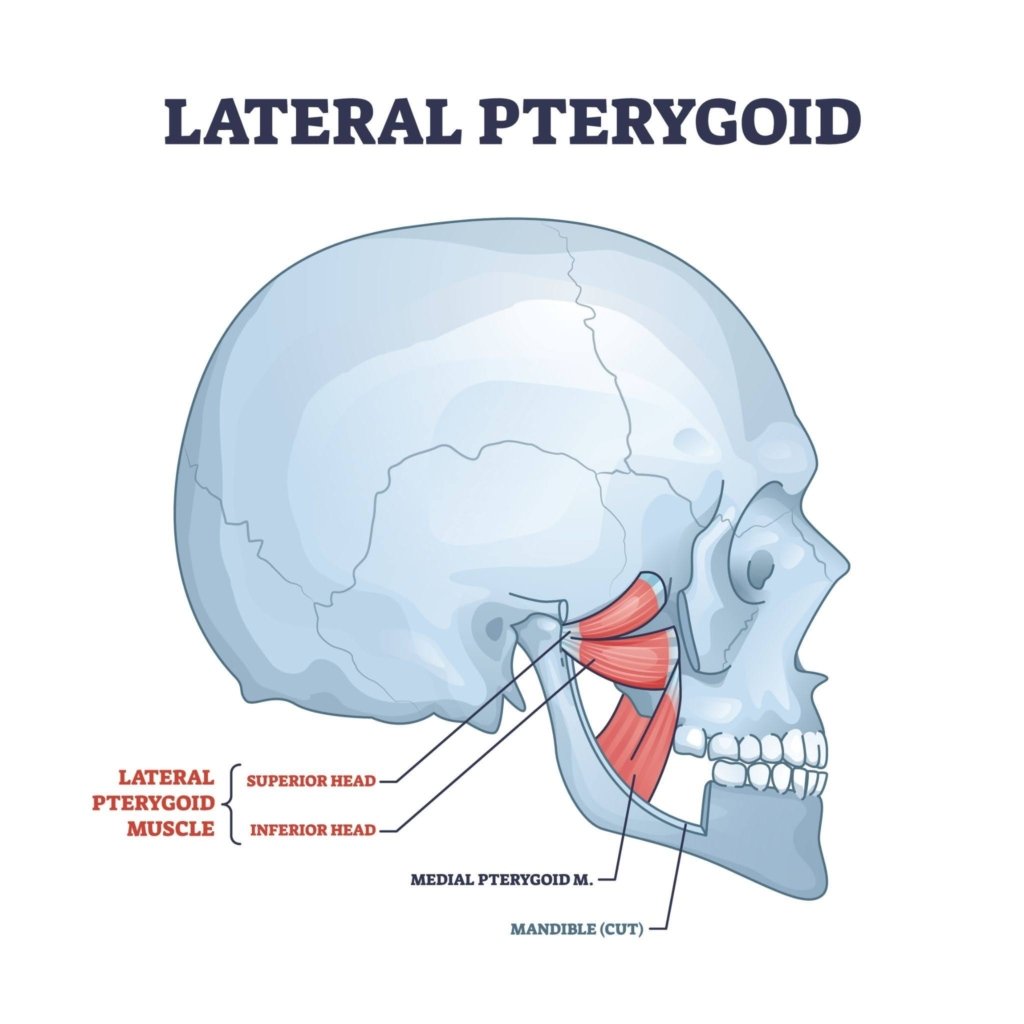
There is an important network of muscles and ligaments that control the movements of the jaw. These muscles are:
- Masseter & Temporalis - These are the big power muscles that help you bite and chew.
- Lateral & Medial Pterygoids - Smaller but equally important muscles that help to stabilise the jaw can control movement.
- Digastric & Mylohyoid Muscles - These muscles help with opening the mouth and swallowing.
If the muscles in the jaw become tight, overactive, or imbalanced, then they can pull the jaw out of alignment, which can lead to altered movement patterns, pain and dysfunction.
What Causes TMJ Dysfunction and Pain?
There’s rarely just a single cause of TMJ issues - it’s often a mix of several factors, which can include any of these below:
- Muscle Overuse - Usually as a result of clenching or grinding your teeth (bruxism); often due to increased stress or anxiety.
- Poor Posture - Having a forward head, chin poking posture (often from desk work or phone use) puts strain on the jaw. This is one of the most common causes of TMJ pain, and is regularly seen in people who have quite a sedentary work life sitting at a computer.
- Cervical Spine Dysfunction - In particular, dysfunction at the C2-C3 level of the spine can contribute to TMJ pain and movement restrictions. The upper cervical spine shares nerve pathways with the TMJ via the trigeminal nerve, meaning irritation or dysfunction at C2-C3 can lead to referred pain in the jaw, face, and even the ear.
- Lifestyle Factors - These may include habits such as chewing gum excessively, biting nails, or even sleeping on one side too much. It’s also quite common in people who have high stress careers or who are in the performing arts or professional singers.
- Dental Issues - Misaligned teeth or an uneven bite can put extra strain on the TMJ. Dental surgery can also cause TMJ problems. Your dentist should check your jaw alignment, and ideally refer to a physio if any issues are picked up.
- Joint Problems - Joint conditions such as arthritis, which causes inflammation or wear-and-tear within the disc and joint can be a factor.
- Trauma or Injury - While this is less common, a direct blow to the jaw, whiplash, or a surgical dental procedure, can cause an acute flare up of TMJ pain.
What are the Symptoms of TMJ Dysfunction?
Symptoms can vary from person to person. They usually come on gradually over time, rather than a sudden onset. People will often feel some mild discomfort, or notice a slight clicking which gets worse over a period of a few weeks or months.
These are a few of the most common symptoms that people present with:
- Jaw pain or tenderness (especially around the cheeks or ears)
- Clicking or popping sounds when moving the jaw
- Difficulty opening the mouth fully (or feeling like it "sticks")
- Tension headaches or facial pain
- Ear pain or a feeling of pressure (without infection)
- Neck and shoulder tension or pain
- A sensation of jaw fatigue after eating or talking
You may feel one or a number of these symptoms at the same time, or they may come on at different times.
Often patients present with an issue somewhere else in the body - like neck or back pain, or tension headaches, but then with further questioning also mention that they have been having jaw discomfort too, which they hadn’t focused on.
What Makes TMJ Pain Worse?
If your symptoms fluctuate or seem to get worse at certain times, you’re not imagining it. Some people find that their symptoms come and go a bit, which is often why they don’t seek help immediately.
Common aggravating factors include:
Stress & Anxiety - If you have a stressful time in your life, it can lead to jaw clenching and teeth grinding (sometimes even in your sleep). Once the stress subsides, so can your pain.
Poor Posture - Sitting for prolonged periods hunched over at a desk or looking down at your phone can exacerbate your symptoms.
Chewing Hard Foods - Things like crusty bread, chewy meats, or gum can make symptoms worse.
Sleeping Position - Sleeping on your front or side with increased pressure on your jaw can add to your pain.
Talking for Long Periods - Public speaking, singing, or even long phone calls can increase your symptoms.
How is TMJ Dysfunction Diagnosed?
At Complete Physio, we take a thorough and structured approach to diagnosing TMJ dysfunction. Understanding the root cause of your symptoms is important to creating the right treatment plan.
That’s why our TMJ specialists carry out both a detailed subjective history as well as a comprehensive objective assessment during your initial appointment.
Subjective Assessment - Understanding Your Symptoms
We’ll start by asking you lots of questions about the following:
- The type, location, and duration of your pain.
- Any clicking, locking, or stiffness in the jaw.
- What activities make it worse or better (e.g., chewing, stress, posture).
- Any history of jaw trauma, dental work, or orthodontic treatment.
- Symptoms such as headaches, ear pain, or neck tension that may be related.
- Lifestyle factors, including stress levels, occupation, sleep habits, and posture at work.
- We’ll also do a full body scan, asking you about any other injuries or niggles that you may feel are unrelated, but help to build up a complete picture of your condition.
Objective Assessment - A Hands-On Approach
Next, we carry out a detailed physical examination, including:
- Jaw Movement Testing - Assessing how far and how smoothly you can open and close your mouth.
- Palpation (Hands-On Examination) - Feeling for muscle tightness, tenderness, or joint irregularities around the jaw, neck, and shoulders.
- Listening for Clicking or Popping - Identifying joint noises that may indicate disc displacement.
- Postural Assessment - Looking at your jaw, head, neck, shoulder and back alignment, as poor posture can contribute to TMJ issues.
- Bite & Dental Screening - Checking for tooth wear, clenching, or grinding habits that may be affecting your jaw.
Diagnosis - Bringing It All Together
From this assessment, we can determine whether your symptoms are muscle-related, joint-related, or a combination of both.
We will then be able to look at what your best treatment options might be, tailored to your specific needs.
You may benefit from physiotherapy, injection therapy, or a referral for further investigations (such as an MRI or a dental consultation).
By combining specialist physiotherapy expertise with advanced diagnostic techniques, we ensure you get a precise diagnosis and a personalised treatment plan.
How Do We Treat TMJ Dysfunction at Complete Physio?
The good news. TMJ dysfunction is highly treatable, and with the right approach, most people see significant improvement. At Complete Physio, we take a comprehensive, evidence-based approach to ensure you get the best possible outcome.
1. Physiotherapy Treatment
Physiotherapy is always the first line of treatment for TMJ pain and dysfunction. Our specialist physiotherapists understand that there’s no one size fits all when it comes to treatment. They will often use a combination of modalities such as:
- Postural correction - To address poor postures that could be causing or contributing to your pain.
- Targeted exercises - To strengthen the jaw and deep neck muscles for long-term relief.
- Hands-on joint mobilisation techniques - This may focus on the jaw or might also include mobilisations to the cervical spine, which is often an area of dysfunction in TMJ patients. To improve jaw mobility and reduce tension.
- Soft tissue massage & trigger point release - To ease muscle tightness and tension in the jaw, neck, and shoulders.
- Relaxation techniques and lifestyle advice - To help reduce anxiety and stress which leads to clenching and grinding.
2. Injection Therapy
If you have persistent, severe pain and symptoms that physiotherapy intervention alone is not alleviating, you may be a good candidate for injection therapy.
We work closely with our medical team to offer ultrasound-guided injections, led by Dr Matteo Bernardotto.
These include:
- Corticosteroid Injections - Corticosteroid works as a very effective anti-inflammatory treatment which will reduce pain in the TMJ.
- Botox Injections - These injections are used to relax overactive jaw muscles and relieve tension-related symptoms.
- Hyaluronic Acid Injections - These can help improve joint lubrication and function.
- PRP Injections - PRP is an injectable solution of a patient's own blood platelets, which are rich in growth factors that promote healing and tissue regeneration - again helping to reduce pain and restore function.
3. Surgical Options
Surgery is rarely needed, and is only ever a last resort; but in severe cases, options include:
- Arthrocentesis - A procedure to flush out debris and inflammatory substances within the joint.
- Arthroscopy - Keyhole surgery to examine and repair joint damage.
- Open Surgery - Reserved for extreme cases where joint reconstruction is necessary.
Why Choose Complete Physio for TMJ Treatment?
- We have specialist physiotherapists with advanced training in TMJ dysfunction
- We offer a unique, holistic, multidisciplinary approach - combining physio & medical expertise, for a seamless treatment journey
- Ultrasound-guided injection therapy can be arranged quickly and easily, for fast, targeted pain relief, without the need for a separate GP referral.
- Personalised care tailored to you and your needs. No one patient is the same, we will ensure that your treatment plan is specific to your symptoms and goals.
At Complete Physio, we have dedicated physiotherapists with specialist training in treating TMJ dysfunction. Our expert team takes a holistic approach, looking at the body as a whole, not just at the area of the jaw.
We know that TMJ pain can be quite complex and your treatment often needs to address multiple factors that might be contributing to your symptoms.
Your treatment will involve combining, posture reeducation, hands-on therapy, tailored strengthening exercises, and, where needed, an ultrasound-guided injection service.
We work closely with pain specialists and consultants, meaning you’ll get a comprehensive, joined-up treatment plan.
References
- La Touche, R., Fernández-de-las-Peñas, C., Fernández-Carnero, J., Díaz-Parreño, S. and Paris-Alemany, A. (2009) ‘The effects of manual therapy and exercise directed at the cervical spine on pain and pressure sensitivity in patients with temporomandibular disorders’, Journal of Oral Rehabilitation, 36(9), pp. 644–652.
- Kalamir, A., Pollard, H. and Vitiello, A. (2012) ‘Intra-oral myofascial therapy versus education and self-care in the treatment of chronic myogenous temporomandibular disorder: a randomised clinical trial’, Chiropractic & Manual Therapies, 20, Article 17.
- Armijo-Olivo, S., Pitance, L., Singh, V., Neto, F., Thie, N. and Michelotti, A. (2016) ‘Effectiveness of manual therapy and therapeutic exercise for temporomandibular disorders: systematic review and meta-analysis’, Physical Therapy Reviews, 21(1), pp. 39–55.